Paragon has much to share this week. Fortunately, they’ve added an extra day to February just to fit it all in. We have op-eds on Medicare Advantage and Medicaid redeterminations, a public comment about association health plans, the weekly Paragon Pic, and we’re hosting a virtual event on Medicare Advantage next week.
Improving Medicare Through Medicare Advantage
Today, Paragon’s senior policy analyst Joe Albanese has an op-ed in the Washington Examiner summarizing the key issues and recommendations from his recent Paragon report.
- These include changes to plans’ benchmarks, quality bonuses, and risk adjustment payments, as well as other provisions to improve parity between MA and traditional fee-for-service (FFS) Medicare.
- The recommended policies would save an estimated $250 billion over ten years.
Joe’s op-ed argues that the growth of MA into the most popular form of Medicare coverage presents a unique opportunity for policymakers:
Patient choice is transforming the entire Medicare program in a way that bureaucrats have been unable to do.
But there are opportunities to improve MA that will allow it to drive even more innovation for more people. To do that, it is necessary to address concerns that overall MA spending is higher than FFS despite MA’s success in lowering health care expenses. This will require refinements to MA’s structure and overdue reforms to FFS.
Joe concludes the op-ed with the recent lesson of the Part D drug program to show why MA’s supporters should not simply be content with the status quo.
Paragon Event on MA Next Week
On Thursday, March 7 at 1pm EST, Paragon will host a virtual discussion of MA and Paragon’s new paper. The discussion will feature Paragon’s Demetrios Kouzoukas and Joe Albanese, Loren Adler of the Brookings Institution, Josh Gordon of the Committee for a Responsible Federal Budget, and Chris Pope of the Manhattan Institute. Register for the event here.
MA Plans Typically Cover Benefits Below Traditional Medicare Costs
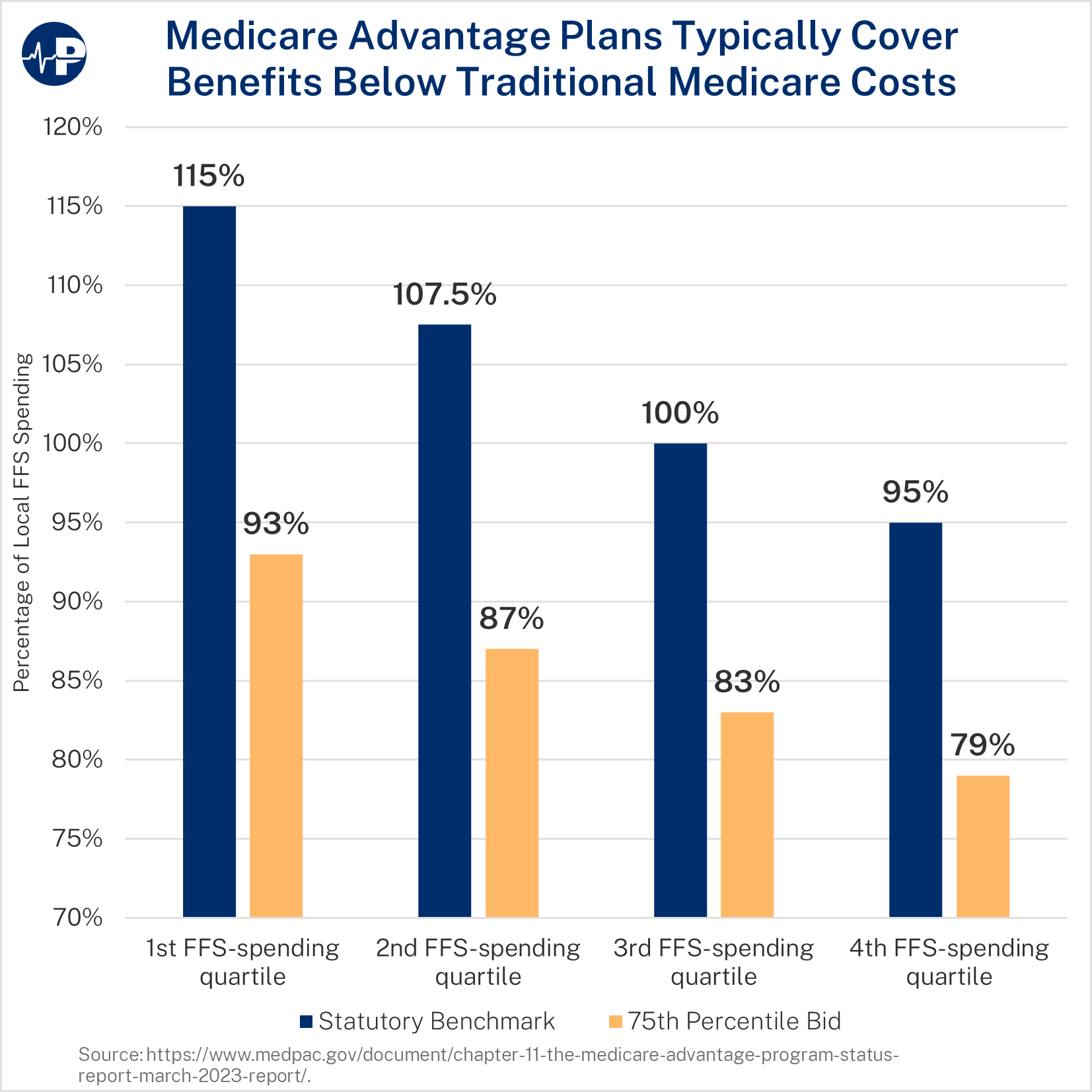
Today’s Paragon Pic, featured below, shows that MA plan bids are typically well below both FFS costs and benchmarks—demonstrating that the vast majority of plans can deliver core Medicare benefits at significantly lower cost than FFS. Find a full analysis of today’s pic here, which shows the statutory benchmark as a percentage of FFS spending by quartile with the 75th percentile MA bid in those areas.
Biden’s Misguided Proposal to Restrict Small Employer Health Options
On February 16, Paragon led a comment letter of several of the nation’s top health policy experts in opposition to the Department of Labor’s (DOL) proposed rule to rescind DOL’s 2018 rule that expanded the ability of employers to offer their workers coverage through an Association Health Plan (AHP). AHPs enable employers to offer high-quality coverage that avoids some costly government regulatory requirements and permits employers to pool their workers to take advantage of economies of scale and improved bargaining power with providers. The Paragon-driven letter points out several problems with the Biden administration proposal:
- DOL mistakenly suggests that AHPs operating under the 2018 rule would be more likely to offer “skinny” coverage.
- DOL mistakenly suggests that AHPs operating under the 2018 rule would promote adverse risk selection and market fragmentation.
- DOL ignores the success of purchasing arrangements analogous to AHPs.
- DOL ignores the costs of rescinding the 2018 rule.
Policymakers should be looking to expand options for small businesses and their workers, particularly given small businesses have increasingly stopped offering coverage after the passage of the Affordable Care Act.
For more on AHPs, see Paragon’s policy brief, Small Business Health Insurance Equity Through Association Health Plans.
Much Larger Medicaid Program Likely a Lasting Effect From Pandemic
On February 27, I posted a new piece at Forbes, analyzing updated data on the Medicaid redeterminations and removal process. Here are two key points worth emphasizing:
- A survey of insurers participating in Medicaid found that they expect to retain about 30% of the pandemic-related Medicaid growth post completion of Medicaid redeterminations.
- Secretary Becerra’s recent letters to states criticizing their redeterminations and removal process were highly political. None of the nine states with the highest percentage of disenrollment for procedural reasons received letters. This includes five states with Democratic governors (New Mexico—93%, California—88%, North Carolina—87%, Washington—86%, and Hawaii—86%) and the District of Columbia with an 89% procedural disenrollment rate. Texas and Florida, which received HHS letters and have attracted a lot of attention, have procedural disenrollment rates of 67% and 60%—below the national average.
Join me at AEI on Friday, March 1st
In closing, I’ll be a participant at a forum at the American Enterprise Institute on Friday from 10-11:30 am EST to discuss the Affordable Care Act’s survival, evolution, and implications for future policy with a very distinguished set of co-panelists. I encourage you to register here.
All the best,
Brian Blase
President
Paragon Health Institute



