Reforming Government, Empowering Patients
Navigation
Pandemic Unwinding
How States Should Clean Up Their Medicaid Rolls


The Paper
This paper outlines strategies for states to efficiently clean up their Medicaid rolls post-COVID-19 by prioritizing the removal of ineligible enrollees, leveraging enhanced federal funding, and providing recommendations to ensure resources are preserved for those truly in need, amidst a backdrop of nearly 20 million potentially ineligible enrollees due to pandemic-era enrollment policies.
Key Takeaways
- The continuous enrollment requirement for Medicaid during the COVID-19 public health emergency has led to upwards of 18 million Medicaid enrollees who do not meet eligibility requirements for the program.
- As of April 1, 2023, states have resumed regular eligibility redeterminations to preserve Medicaid for those who truly need the program and to protect taxpayers. States should prioritize resources and start with reviews of those most likely to now be ineligible.
- States have an incentive to act expeditiously, as enhanced federal COVID funding for Medicaid has already begun winding down and will be gone by the end of 2023.
- The vast majority of people enrolled in Medicaid who are ineligible already have other sources of coverage or will transition to other sources of coverage when their Medicaid enrollment ends.
- There are numerous protections for people who are removed from the program and who are still eligible, including retroactive Medicaid coverage that pays for three months of past medical expenses.
GROWTH OF INELIGIBLE MEDICAID ENROLLEES
During the Obama and Biden administrations, the federal government relaxed Medicaid eligibility requirements, making it easier for millions of ineligible individuals to access the program and more challenging for states to verify applicant information and ensure that only those eligible were enrolled.1 This has contributed to the program’s significant expenditure growth and surge of improper payments over this period. Further, coverage of those who do not qualify for Medicaid crowds out private coverage—particularly employer-sponsored insurance—and shifts costs to taxpayers.2 All of this depletes resources for more vulnerable populations that need a safety net. Prior to the COVID-19 public health emergency (PHE), Medicaid’s improper payment rate already exceeded 20 percent, or nearly $100 billion in federal misspending annually.3 The high improper payment rate was driven by improper eligibility reviews, largely resulting from the incentives for states to enroll people as eligible under the Affordable Care Act (ACA) expansion to obtain a higher federal reimbursement.4 Congressional action at the beginning of the COVID-19 pandemic made the problem worse.
Through the Families First Coronavirus Response Act, Congress offered states enhanced Medicaid matching funds (a 6.2 percentage point boost for traditional Medicaid enrollees) for the duration of the PHE so long as states did not make eligibility reductions or remove ineligible enrollees from the program. While states had the option to not take the funding or to opt out early, all states accepted the funds and did not remove ineligible Medicaid enrollees for more than three years. The continuous coverage provisions after the precipitous employment decline led to many millions more people on Medicaid who returned to the workforce relatively quickly. As a result, nearly 20 million people now have two sources of coverage, with the most common being employer coverage and Medicaid.5
The congressional spending bill passed at the end of 2022 changed the terms of this agreement with states. As of April 1, 2023, states are allowed to resume full eligibility reviews without the risk of losing enhanced federal funding. States are incentivized to start doing redeterminations as quickly as possible as federal funding has also begun ratcheting down and will continue dropping throughout the remainder of the year.
Ultimately, Medicaid misspending harms Americans by taking limited resources from those who rely and depend on these programs—reducing their access to care. Many of them, such as low-income children, pregnant women, individuals with disabilities and the elderly, need Medicaid to finance their medical services.
Medicaid is the nation’s largest public welfare program, costing nearly $800 billion in federal and state funds annually. Medicaid is the largest spending category in state budgets.6 The PHE’s continuous coverage policy drove enrollment even higher, adding nearly 20 million people to Medicaid and creating many program integrity issues.7 Medicaid now has more than 86 million enrollees.8 Approximately 18 million of these recipients are likely to be ineligible for Medicaid.9 An alternative enrollment methodology by the Centers from Medicare and Medicaid Services (CMS), which includes people enrolled in limited benefit plans and counts people enrolled at any time during each month in the quarterly reporting period, suggests that enrollment was around 94 million people in September 2022.10
Pre-pandemic data also showed that one in 10 Medicaid recipients were transient and changed addresses often.11 Movement to another state would result in ineligibility within the previous state, a problem that has not been corrected since early 2020 as states have not reviewed eligibility. The Public Assistance Reporting Information System (PARIS), which assists eligibility workers nationwide to identify recipients with multi-state enrollment, was suspended during the PHE because redeterminations were halted.12 A recipient who is enrolled in Medicaid in multiple states that both use managed care organizations (MCOs) means that two MCOs are receiving capitation payments for this one recipient.13 An analysis from the Urban Institute estimates that 99 percent of individuals expected to be removed from Medicaid through the redeterminations will be eligible for employer-based coverage, ACA exchange subsidies, or other taxpayer-funded coverage such as the Children’s Health Insurance Program (CHIP).14
STATES SHOULD ACT EXPEDITIOUSLY TO PROPERLY REDETERMINE ELIGIBILITY
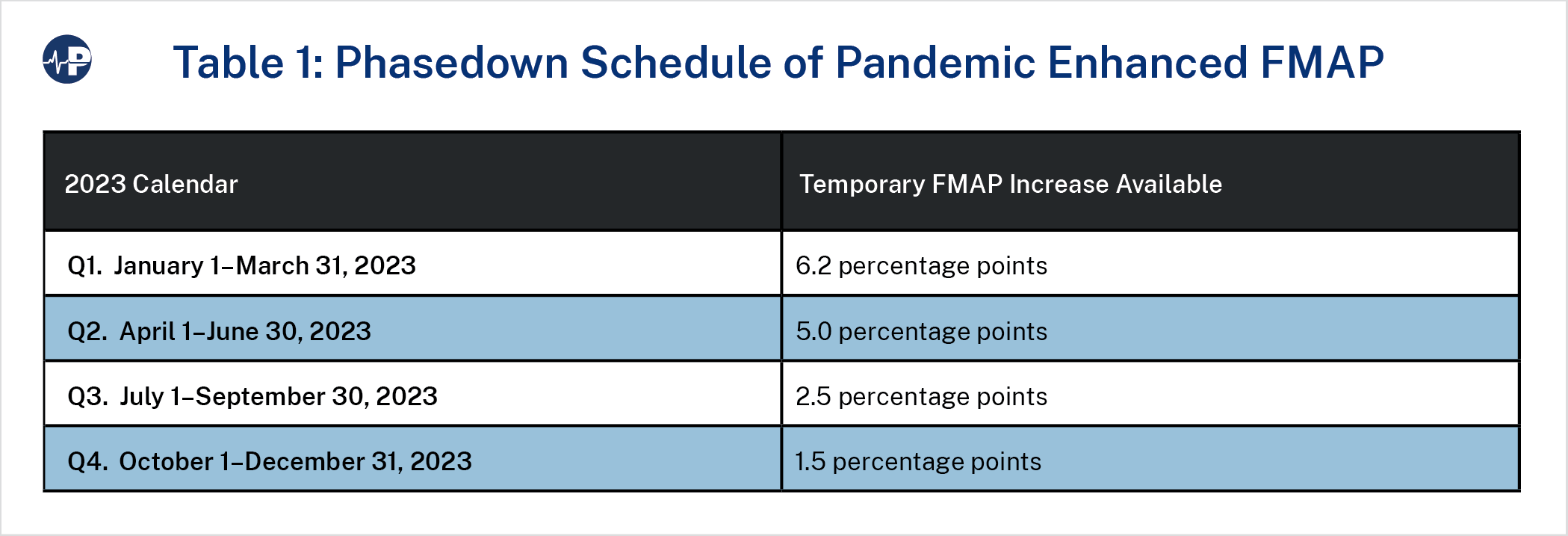
The enhanced funding associated with the continuous coverage requirement (a boost in states’ federal medical assistance percentage, or FMAP) has already begun phasing down and will end entirely at the end of 2023. As of April 1, the enhanced federal funding dropped from 6.2 percentage points to 5.0 percentage points. On July 1, it will drop again to 2.5 percentage points and to 1.5 percentage points in the fourth quarter of the year. The phase-down and end of the enhanced FMAP means states have an incentive to ensure that as many ineligible enrollees are removed by the end of the year. States, therefore, need to quickly create a roadmap that removes the ineligible enrollees expeditiously and preserves resources for the truly needy.
The reinstated eligibility redetermination process will present states with some challenges due to the myriad of newer eligibility rules that make it easier to attain and maintain eligibility, potential staffing shortages, and many recipients’ unknown or unreported mailing addresses.16 These rules, which impose burdens on states that must be met before anyone can be removed from Medicaid, are intended to ensure that Medicaid-eligible recipients stay on the program and to protect those who might be incorrectly removed. These new rules are a reversal from longstanding eligibility rules, including in President Obama’s first term, which allowed states to perform eligibility reviews and verifications every six months or even more often, required a minimum of one such review per year, and included strict income verification guidelines. Moreover, those removed from the program incorrectly can easily regain access to Medicaid. The totality of these new rules and enrollee protections should shield states from accusations of moving too fast to ensure that only those eligible are enrolled. For example, before anyone can be removed, states must:
- Attempt to obtain current contact information for recipients;17 and
- Make a good-faith effort to contact recipients via different methods if they have their mail returned.18
For individuals who might be incorrectly removed, there are also many protections, including but not limited to:
- Retroactive eligibility: Individuals who qualify for Medicaid can enroll and have their medical expenses covered by taxpayers retroactively so long as they were eligible when the services were received. If individuals are incorrectly removed, they can re-enroll in the program and still have their expenses covered, with up to three months of expenses paid by Medicaid.
- Hospital Presumptive Eligibility (PE): If there is a medical necessity, a disenrolled person can reapply for the program the day after coverage expires through PE. PE is an expedited Medicaid application process through the hospital that permits a Medicaid determination based on only a few questions about income and household size and without verification. If individuals meet these basic and initial requirements, they are immediately presumed Medicaid eligible. They receive temporary coverage pending completion of a full eligibility review. This means that a person who is disenrolled often finds it easy to get back on the program through PE when receiving medical services.19
- Testing each Medicaid eligibility group: When individuals apply for Medicaid, eligibility workers must test their eligibility under each enrollment category. If a current recipient is found not eligible under the requirements for his or her original enrollment category, the state is required to test eligibility under the requirements to see if he or she meets eligibility for any other enrollment category. The state must exhaust all Medicaid enrollment categories and give the applicant every possible chance to become eligible.20 For each group there are numerous statutory and regulatory “pathways” for establishing eligibility. Each pathway is defined by specific income and resource requirements that are determined by each state within federal guidelines. Some of these pathways apply in all states. As an example, if a childless adult is redetermined and is found ineligible, “the Medicaid agency must consider whether the recipient may be eligible under one or more other eligibility groups covered by the state.”21 In the current unwinding process, if enrollees are incorrectly removed, they can simply reapply for coverage and states will be compelled to test them for eligibility in all other Medicaid categories.
- Fast-track eligibility: Newer federal rules initiated by Presidents Obama and Biden allow Medicaid applicants to become eligible for the program and stay eligible in a more expedited fashion than traditionally allowed. This has been called fast track or express lane eligibility, and it requires that states review eligibility no more than once per year, permit ex-parte renewals,22 using prepopulated forms from older data—instead of requiring recipients to fill out new forms—and allow self-attestation of many characteristics like income.23 After reviewing all of this information, if the state decides that the information is inadequate to verify eligibility, it must provide the applicant at least 90 days to respond from the date of the eligibility request. If the applicant is ultimately found ineligible, the state would have made three or more months of improper payments with little ability to recoup the benefits.
- Medicaid appeals process: Lastly, if recipients are removed, they are entitled to an extensive appeals process. These appeals can be filed up to 90 days after enrollees are notified about the termination of their enrollment. In many cases, filing an appeal can preserve an enrollee’s benefits until a decision is reached.24
These are just some of the protections in place that protect Medicaid enrollees from wrongful disenrollment. Some states are even taking additional steps to minimize the chance of disenrolling eligible individuals.25 Overall, existing Medicaid rules and regulations provide ample protection for enrollees, and misguided fear should not deter states from moving swiftly to conduct redeterminations and best ensure taxpayer funds are preserved for those eligible.
VAST MAJORITY OF PEOPLE REMOVED FROM MEDICAID WILL OBTAIN OTHER COVERAGE
Almost all current Medicaid enrollees who do not meet eligibility requirements either already have other coverage or will qualify for it once they lose Medicaid. According to the Urban Institute’s estimates, 18 million people will lose Medicaid once redeterminations are completed.26 Nearly 10 million of them will transition to employer coverage, with many of these individuals currently dually enrolled in employer coverage and Medicaid. According to Urban, more than 3 million children will transition from Medicaid to CHIP, and 1 million people will move to nongroup coverage. Additionally, Urban estimates that 40 percent of those disenrolled who would lack coverage will qualify for low- or no-cost coverage on the ACA insurance exchange, which is heavily subsidized by taxpayers. Moreover, some people who are eligible for programs do not enroll. According to an earlier Urban study that focused on eligibility for other programs for those no longer eligible for Medicaid, only 1 percent of removed enrollees will not qualify for other forms of subsidized coverage, including employer coverage, when they lose Medicaid eligibility.27
Many improperly enrolled individuals are also likely now to be enrolled in multiple states. For example, the Medicaid CHIP Payment and Access Commission found pre-pandemic that 6 percent of enrollees were enrolled in multiple states.28 These individuals should be removed from states they no longer reside in but could retain eligibility in their current states, assuming they meet other eligibility criteria.
STATES DO NOT RISK LOSING ANY FEDERAL MONEY FROM EXPEDITING REDETERMINATIONS
Despite some misimpressions, there are not any negative repercussions to states for quickly processing redeterminations. In guidance on how to re-instate the redetermination process, CMS recommended that states “initiate no more than 1/9 of their total caseload of Medicaid and CHIP renewals in a given month during the unwinding period.”29 However, this timing is not a requirement. Further, states are not at risk of losing the enhanced funding sooner than the end of the year if they move more quickly so long as they comply with other federal requirements.30
As discussed, states have an incentive to move quickly, because the enhanced federal funding has already been reduced and will expire at the end of 2023. Indeed, the longer states wait to remove ineligible enrollees from the Medicaid rolls, the more they will pay out of their own budgets to cover them.
Case Study: Lessons Learned from Arkansas’s Redeterminations Approach
Although Arkansas did not remove ineligible enrollees during the PHE, the state continued doing regular eligibility reviews throughout the past three years. This has allowed the state to update and collect data on existing enrollees, flag enrollees who had subsequently become ineligible, and verify that they had reliable contact information for enrollees. This proactive work has made it significantly easier for the state to resume the full redetermination process.
According to the Arkansas Department of Human Services (DHS), as the state begins preparing for redeterminations, it is prioritizing “those whose coverage has been conditionally extended due to the PHE.”31 In other words, because state workers have been consistently reviewing cases for the past three years, they know which enrollees lost eligibility but were extended nonetheless because of the continuous eligibility requirements.
In January 2023, Arkansas began connecting with long-term care facilities and conducting redeterminations. This population is perhaps the least likely to face eligibility changes and also requires the least amount of follow-up for verification. In addition, in February 2023, Arkansas began reviewing cases of able-bodied, working-age adults. These individuals are perhaps the most likely to have experienced changes, such as earning higher income, that would affect their eligibility given that they are in their prime working years and many of them may have become eligible for Medicaid in the first place due to pandemic-induced job loss.
Arkansas is also resisting the ACA’s perverse funding incentive to target traditional Medicaid enrollees for redetermination. Because the federal government pays a much higher share of the costs of ACA expansion enrollees, states have a financial incentive to redetermine traditional Medicaid enrollees first.32 Doing so would save them more state dollars than removing ACA expansion enrollees would, because federal taxpayers pay much less for the traditional populations, who also tend to be more expensive.
REDETERMINATIONS ROADMAP: RECOMMENDATIONS FOR STATES
Here are seven steps that states should take to perform expedited and efficient redeterminations.
- Prioritize reviews for those most likely to be ineligible. To move through the caseload expeditiously, states should use the following list for prioritizing the categories of recipients for redeterminations:
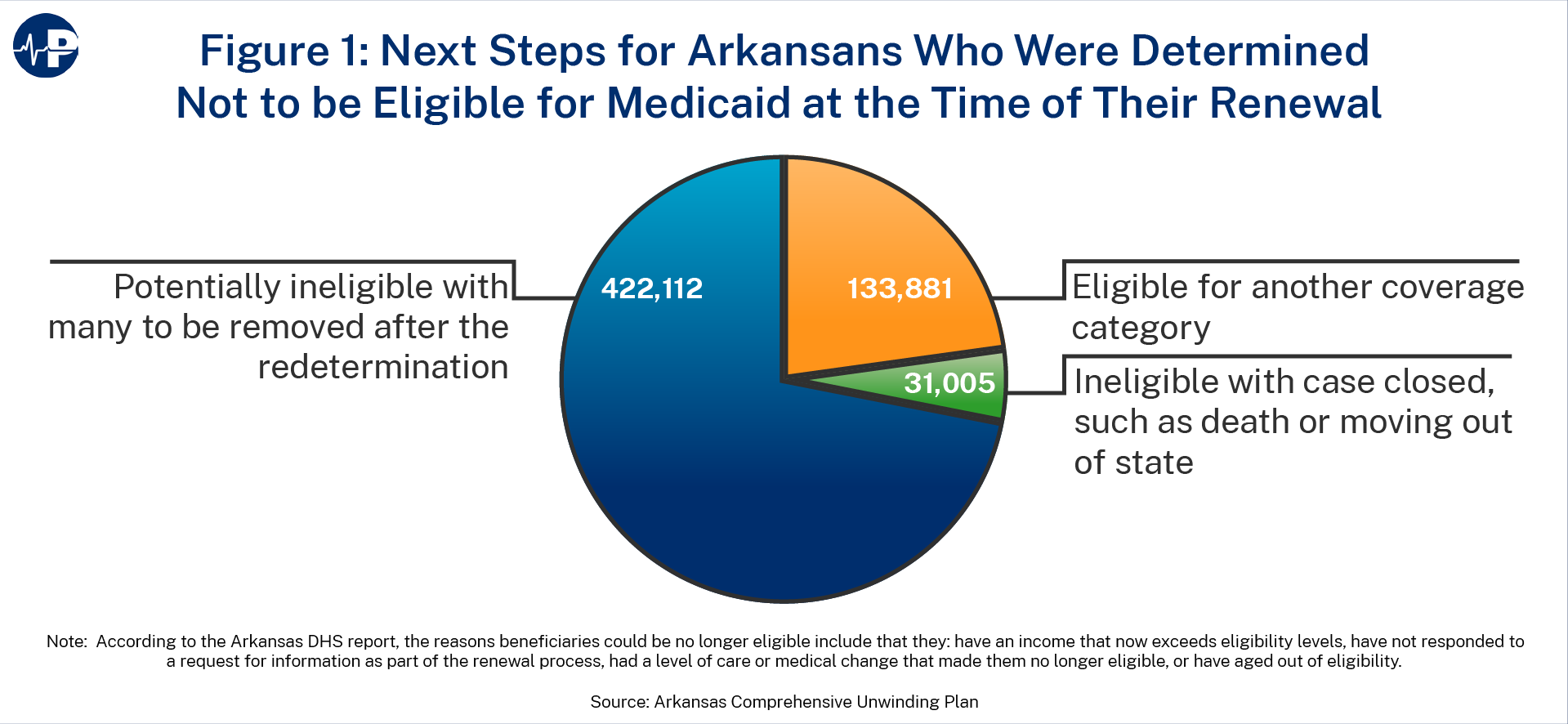
- Enrollees for whom the state has received information indicating a change in circumstances, such as a change in residency, employment status, or income. According to Arkansas DHS, there are roughly 422,000 such individuals in Arkansas.33
- Enrollees for whom the state has outdated information or whom the state has not been in touch with for the past few years. Many of these enrollees might have been working at the beginning of the pandemic, and their incomes nearly exceeded the eligibility income limits prior to the PHE, or their incomes have subsequently significantly increased.
- Individuals identified through claims data as not having recently used services. If someone is enrolled in Medicaid, principally through a Medicaid managed care plan, and has not used medical services over the past 12-month period, he or she likely has another form of insurance and is no longer eligible for Medicaid.
- All other non-disabled enrollees because they are most likely to experience frequent changes in circumstances.
- Categorically ineligible recipients. After turning 19, in many cases, enrollees might lose their eligibility for Medicaid and CHIP and are subject to the more limited Medicaid eligibility criteria for adults. Most near-elderly Medicaid enrollees who then turn 65 should be removed from Medicaid.
- Everyone else.
- If recipients do not respond, close the case. State Medicaid agencies must send the enrollee a notice of the information that the enrollee must provide, giving the enrollee 30 days to respond. If the enrollee does not respond within the 30 days, the state should send a letter terminating coverage. If the enrollee provides information prior to the deadline and the information shows the person is no longer eligible for the program, the state should give a 10-day notice before terminating enrollment.34
- Organize staff properly and ensure adequate resources. States and counties that are short-staffed should consider hiring retirees or contract workers on short-term or part-time contracts for the rest of 2023 to help process redeterminations more expeditiously as well as to be prepared for an expanded number of appeals.35 Further, states should consider organizing special units in county or field offices where staff can quickly review certain categories of enrollees. This would help to focus efforts and set achievable monthly goals. Program integrity staff should be integrated where possible to ensure that efforts focus on reducing fraud and wasteful spending.
- Resume using PARIS. As discussed above, PARIS should be reinstated as part of the eligibility process now that the PHE has ended. PARIS assists eligibility workers nationwide to identify recipients with multi-state enrollment. This system was suspended during the PHE.
- Ensure frequent data matches to identify third-party liability.36 Medicaid should be the payer of last resort if the person has another source of coverage. Many ineligible recipients have dual coverage, in which they are enrolled in both Medicaid and employer-sponsored insurance. Given the surge of able-bodied adult enrollment that occurred in Medicaid during the COVID-19 pandemic and the large increase in unemployment at the beginning of the pandemic, this focus is even more important as many of these working-age adults have gone back to work and have obtained, or are eligible for, employer-sponsored health insurance. If the recipient does not report another form of insurance, federal rules require states to perform matches with income and workers’ compensation databases and motor vehicle accident files in the state to determine if the government is due third-party liability payments.37 The state may also perform matches with other potential sources of coverage, such as the Department of Defense (DOD). Medicaid enrollees or dependents may also be on DOD plans.38 Matches such as this help the state recoup inappropriate funds expended through Medicaid.
- Establish links to credit bureaus and other state agencies. States can also verify eligibility by linking to credit bureaus and other state agencies such as departments of revenue and workforce services. These will be important to verify residency, income, and employment.
- Use enhanced data and artificial intelligence (AI). States should also consider using advanced data analytics tools and AI to help identify patterns that suggest misenrollment.39 Data analytics would help produce lists of likely ineligible recipients that can be shared with staff to expedite redeterminations.
PROTECTING THE VULNERABLE AND TAXPAYERS
The COVID-19 pandemic and the continuous Medicaid enrollment provisions enacted by Congress have led to a surge of Medicaid enrollment and spending. Ineligible and improperly classified Medicaid enrollees was already a massive program integrity problem prior to the pandemic because of the ACA. There are now nearly 20 million people enrolled in Medicaid who are not eligible for the program, almost all of whom have access to another source of subsidized health coverage. States have an obligation to move as quickly and smartly as possible to begin cleaning up their Medicaid rolls. Doing so would represent an important first step toward rebuilding public trust, protecting taxpayers, and preserving resources for the country’s most vulnerable.