Medicare Advantage (MA) plans receive payments from the government to provide health care coverage for their enrollees. These payments are calculated using a complex bidding process. Data from these bids suggest that MA plans are usually more efficient than traditional fee-for-service (FFS) Medicare.
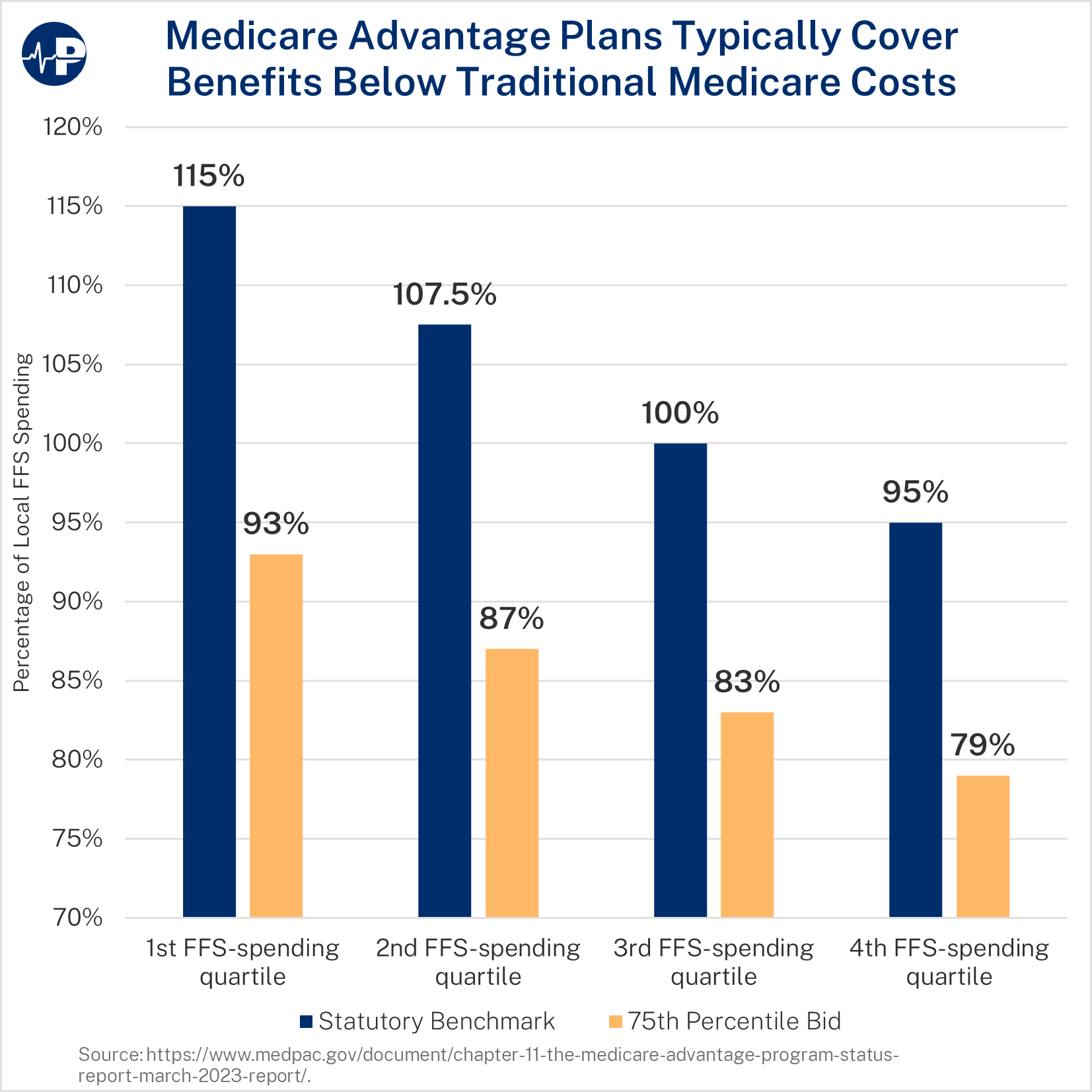
Each MA market area (usually a county) receives a “benchmark” that corresponds to the level of FFS spending in that area. There are four benchmark levels under current law: 95 percent, 100 percent, 107.5 percent, and 115 percent of FFS spending. The lowest quartile of counties in terms of FFS spending receives benchmarks of 115 percent, the second lowest quartile receives 107.5 percent, the second highest receives 100 percent, and the highest receives 95 percent.
Plans submit a “bid” that reflects the expected cost of covering Part A and Part B benefits. If a plan bids above its benchmark, then the government sets its payment at the benchmark and requires it to collect the difference through additional premiums. If a bid falls below the benchmark, the difference is split between the government and a “rebate” that the plan must use to reduce its premiums or provide supplemental benefits.
In 2023, bids were 83 percent of FFS costs on average. In each county quartile, bids at the 75th percentile ranged from 79 to 93 percent of FFS costs—demonstrating that the vast majority of plans can deliver core Medicare benefits at significantly lower cost than FFS. These efficiencies present policymakers with an opportunity to achieve targeted savings in MA without compromising access to benefits or coverage options.
Capping MA benchmarks so that they cannot exceed 100 percent of FFS costs – at least in areas where access to MA coverage is not a concern – would pass along more savings to taxpayers. Most plans would continue receiving rebates to provide extra benefits. Paragon proposes to pair these changes with other policies to improve the accuracy of its benchmark calculations by using only cost data from individuals who .