As we approach the 14-year anniversary of the Affordable Care Act, the law is quite different from what Congress originally enacted and has turned out to be enormously profitable to the health care industry, particularly insurers. Major subsidies to insurers, such as the law’s Medicaid expansion and premium tax credits for exchange plans, are significantly growing while the major provisions that they disliked—the Cadillac tax, the health insurance tax, and the Independent Payment Advisory Board—have been repealed.
In fiscal year 2023, federal subsidies through the ACA Medicaid expansion and the exchanges, which almost all flowed to insurers, totaled $218 billion. About half of all health care spending and the majority of health insurer revenue now comes directly from the government. While private health insurance can provide financial protection and manage risk, the design of the ACA has led to inflationary premiums and spending, often with little value to patients, and has led the industry to be even more reliant on government.
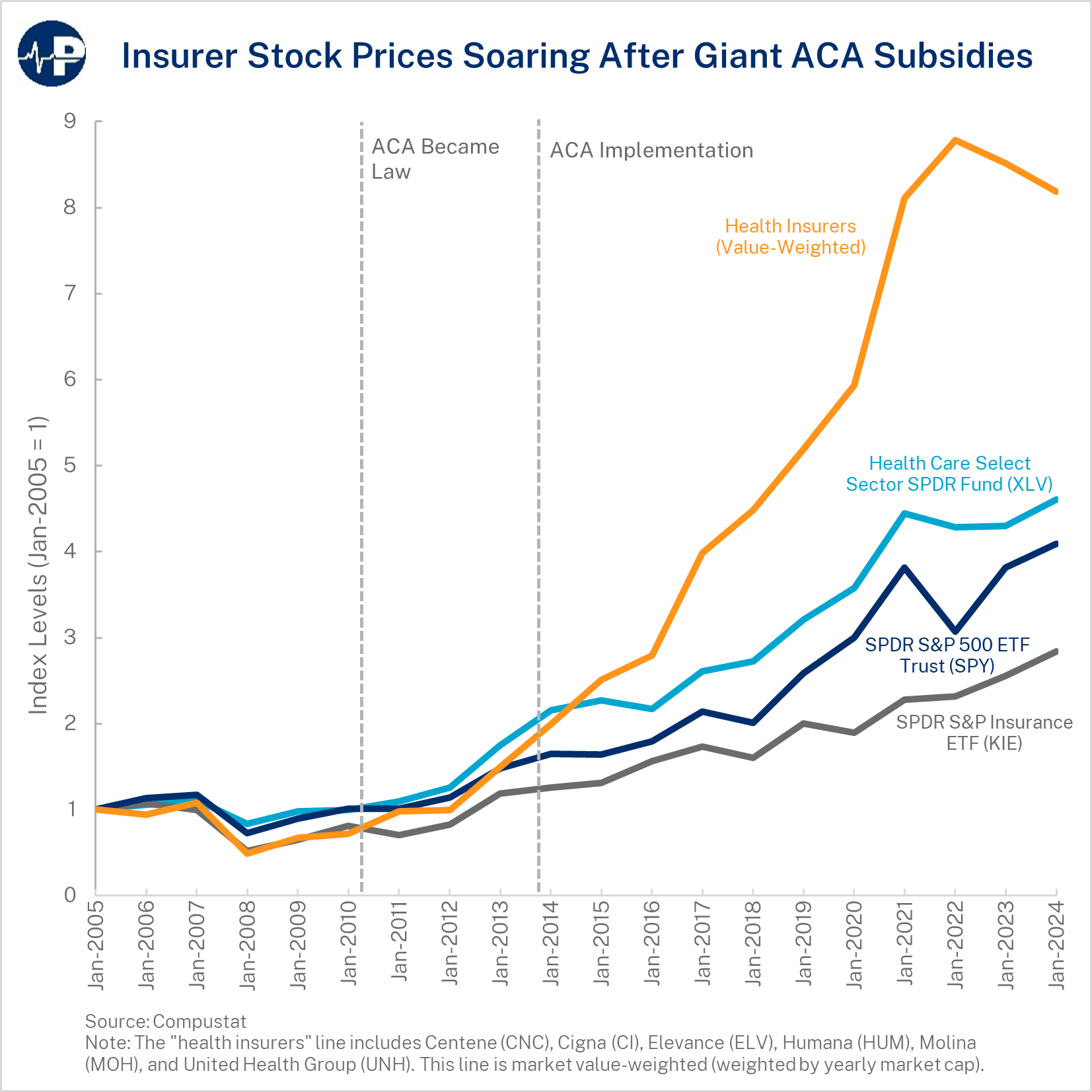
As the Paragon Pic shows, the weighted average of health insurer stock prices are up 1,032 percent from 2010, when the ACA was enacted, and 448 percent from 2013, the year before implementation of the ACA’s key provisions. By comparison, the average respective growth of the most popular S&P 500 exchange-traded fund (ETF) was 251 percent and 139 percent. ETFs are actively-traded funds that own a basket of securities. They often try to track the financial performance of an index, such as the S&P 500 or a specific sector of the economy.
The figure shows the trends over time for the S&P 500 ETF (navy blue), a general health care ETF (light blue), a general insurance ETF (gray), and a market value-weighted group of health insurer stocks compiled by Paragon (orange). Generally, the four industry categories tracked each other closely prior to the ACA taking effect. However, a large divergence appeared once the ACA was implemented, with the health care fund, and particularly the group of health insurer stocks, surging.
Insurers getting windfalls from the ACA’s Medicaid expansion
The ACA’s Medicaid expansion has produced a windfall for health insurers, with federal spending on expansion enrollees equal to $126 billion in 2023 per CBO (the state share would add about another $13 billion). Through the ACA, the federal government pays nearly the entire cost of Medicaid expansion enrollees, and most enrollees are covered by Medicaid managed care, where insurers provide coverage. Since states are almost entirely using federal dollars, they set very high payment rates to insurers for Medicaid expansion enrollees. In inflation-adjusted dollars, Medicaid spending on insurers more than quadrupled from 2010 to 2021. Insurers have also benefited from porous state eligibility determinations that have led to millions of people being placed in a Medicaid managed care plan who are not eligible or without proper eligibility reviews.
Here’s how the Los Angeles Times put it: “Medicaid is rarely associated with getting rich….But some insurance companies are reaping spectacular profits off the taxpayer-funded program in California, even when the state finds that patient care is subpar.”
The main insurers that participate in Medicaid managed care—Molina and Centene—have experienced very large upswings in their stock prices between January 2013 and 2024. Molina is up more than 1,000 percent, and Centene is up more than 425 percent.
Insurers reaping benefits of massive subsidies through the ACA exchanges
The ACA created large subsidies that insurers receive on behalf of most people who enroll in an exchange plan. In essence, the ACA turned the unsubsidized individual market into a market with much higher premiums that people typically need massive subsidies to afford. These subsidies give insurers significant pricing power as the burden of premium increases over time is almost entirely borne by taxpayers. CBO estimates these subsidies equaled $92 billion in 2023. President Biden signed legislation that significantly expanded these subsidies, essentially creating zero-premium plans for many enrollees and making the subsidies available to some households that earn in the top 5 percent of all household income.
Government will continue to subsidize health care for lower-income Americans, but the ACA subsidies need reforms that limit open-ended government commitments and reduce insurers’ substantial pricing power. Reforms, such as Paragon’s HSA option proposal, should also aim to directly assist the individual to enable them to purchase the care that best meets their needs and so providers better meet the demands of patients, rather than those of third-parties.
No results found.