The No Surprises Act, legislation enacted to cure surprise medical bills, is not working as intended and is likely raising health care expenditures. Understandably, Congress wanted to protect insured patients from excessive costs in two situations: 1) in medical emergencies and 2) when they go to in-network facilities but receive treatment from a provider who is out of their network. In both cases, Congress limited patient cost-sharing to no more than they would owe for receiving in-network services.
Rather than leaving insurers and providers to settle on the price for services in which there was no prior contractual arrangement, Congress opted for an arbitration system—so-called independent dispute resolution (IDR). This led to the creation of a new bureaucracy through the Department of Health and Human Services in which the federal government is now a party to resolve payment disputes.
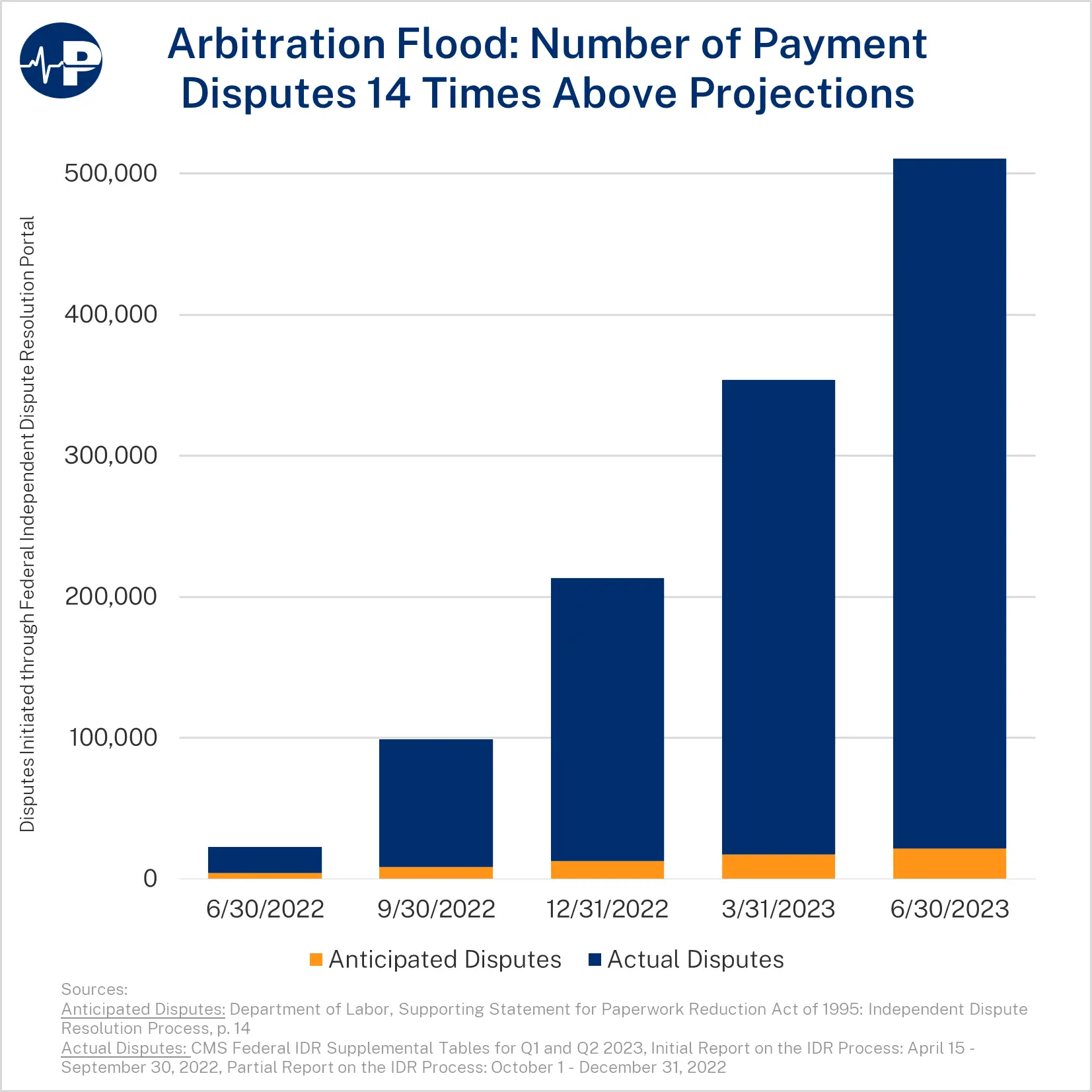
As the figure below shows, there has been a flood of cases submitted to IDR. Here is HHS’s own description:
In the first year … disputing parties submitted 14 times the number of disputes that the Departments had expected to receive in an entire calendar year. Due to this unexpectedly high volume, the limited number of certified IDR entities, the complexity of determining disputes’ eligibility for the Federal IDR process, and a large number of ineligible disputes submitted, it is taking certified IDR entities longer than the timeframes established … to process payment disputes.
In addition to an overwhelming flood of cases, the selected prices are much higher than expected. According to a new Brookings Institution review, the median IDR decision is nearly 4 times what Medicare would pay and the median decision is at least 50% higher than historical mean in-network commercial prices.
Unfortunately, much of what the federal government does in health policy does not work as politicians intend—almost always to the detriment of American families. It appears that The No Surprises Act is no exception. Early evidence shows it will increase what Americans pay for health care, largely through higher insurance premiums, while adding additional administrative complexity to an already too complicated payment system.
No results found.