Reforming Government. Empowering Patients.
Navigation
Long-Term Care: The Solution


The Paper
This paper proposes reforms to reduce dependence on Medicaid and free up private financing to fix the LTC challenges.
Executive Summary
What This Paper Covers
How to pay for aging Americans’ long-term care (LTC) is a difficult policy problem. This paper follows “Long-Term Care: The Problem,” in which I explained how well-intended government policy caused many of LTC’s problems. Too many people end up on Medicaid, which pays too little to ensure access to quality home care and causes excessive reliance on institutionalization and unpaid help from families and friends. In this paper, I propose reforms to reduce dependence on Medicaid and free up private financing to fix the LTC challenges.
What We Found
When people encounter high LTC costs later in life, they typically qualify more easily for Medicaid than commonly thought. This moral hazard discourages early LTC planning. The past policy approach of generous Medicaid LTC eligibility with estate recovery after death did not adequately promote proper planning, either through savings or insurance. Most Americans possess enough wealth to fund their average LTC needs, which is about two years of homebased services. If the average 65-year-old had $70,000 set aside for LTC, it would grow to meet that need after age 85, when LTC commonly occurs. Positive incentives to plan early and pay privately avoid the loss of freedom and high economic cost from compulsory, payroll-funded policies.
Why It Matters
With the aging of the baby boomers and an increasing percentage of the population living past 85, creating a sustainable LTC policy is crucial. If Medicaid did not pay for expensive LTC after care is needed, more consumers would prepare privately and avoid Medicaid dependency. Unless policy is changed and the incentive to avoid proper LTC planning is removed, the LTC system will fail, harming those who most need public support.
Policy Suggestions
Medicaid LTC should be restored as a safety net for indigent elderly people. Lawmakers should eliminate the ability to access publicly funded LTC while preserving wealth. This paper details seven options to empower younger and middle-aged Americans to meet a new, publicized individual LTC planning responsibility. This would unleash wealth currently unused for LTC that remains locked in home equity, individual retirement accounts, life insurance, and estates and reorient the LTC system to cater to seniors’ desires to age in their homes rather than in institutions.
Abstract
As explained in my previous work for the Paragon Health Institute, “Long-Term Care: The Problem,”1 public financing and regulation—principally through Medicaid2—caused most of the problems with long-term care (LTC). Those problems include dubious access and quality, nursing home bias, too little home- and community-based care, inadequate provider revenue, reduced private financing from insurance, savings or home equity, caregiver shortages, excessive emotional and financial strain on family caregivers, and systemic racism.3 Ignoring this causal connection between Medicaid and LTC’s problems, many analysts recommend increasing the government’s role, including by means of a new compulsory payroll-financed social insurance program. But adding even more of the government funding and regulation that caused LTC’s problems would only make these problems worse.
The main components of a better solution are already in place. Personal, not public, responsibility for LTC is deeply rooted in American values, statutes, and policy. Medicaid is the largest LTC payor, but it is not a social insurance program like Medicare. Employees and employers do not contribute a payroll tax to finance it. Medicaid, rather, was intended as the payor of last resort for people who cannot live independently without LTC services and supports but lack sufficient personal funds to purchase them. For decades, federal policymakers of both parties tried to ensure that scarce Medicaid LTC resources went solely to the needy. They failed, leaving Medicaid, including state and federal budgets, financially overwhelmed and most people, regardless of their economic condition, using public assistance if they incur catastrophic LTC costs. The proper goal of public policy remains to target Medicaid benefits to the truly needy and to divert middle-class and affluent people to private financing alternatives. Achieving that goal would deliver a higher quality LTC system that meets patients’ needs and improves care both for those able to pay and for those who need a safety net. The key question remains: How can policymakers reconfigure LTC financing policy to ensure that scarce public resources reach only those most in need?
Congress should remove Medicaid as an end-of-life, wealth-preserving, fail-safe for the middle class and affluent. Medicaid should not reward people who neglect to plan responsibly for LTC by both paying for services and providing asset protection. New public policy should incentivize early planning for LTC that employs private wealth, including savings, home equity, life insurance, and a revitalized private LTC insurance market. Recent research documents lower risk of severe LTC expenses and indicates that consumers have more funds available to pay privately for LTC than previously believed. These facts suggest a way to revitalize the senior living market financially to the benefit of LTC consumers and providers alike. With more private LTC financing, fewer people will become dependent on Medicaid. Medicaid can then become a better payer of last resort than it is now. This paper explains how and why this new approach is plausible, practical, and preferable given current demographic and financial conditions.
THE LTC SOLUTION
In “Long-Term Care: The Problem,”4I described the lessons of LTC history. Public programs have paid for most expensive LTC since 1965. Government policies diverted the public from early private LTC planning and left too many people dependent on welfare-financed nursing home care. Private sector entrepreneurs interceded repeatedly with preferred options such as assisted living, private home care, and insurance. But the dominance of Medicaid and Medicare financing for nursing homes prevented alternative modes of LTC service delivery and financing from fully developing based on consumer preferences. Given the damage government financing and interference have caused, what are the best LTC policy options going forward?
America’s many LTC service delivery and financing problems are understandable, manageable, and correctable. The fundamental issue is that people do not plan, prepare, save, invest, or insure early enough to be able to pay for LTC when they need it, usually much later in life. The current challenge facing policymakers is twofold: (1) how to get people to think about and plan for LTC in their younger, working years, when LTC risk and cost seem distant and low compared to more immediate needs, and (2) how to provide and pay for LTC in the future for burgeoning numbers of aging people who are unprepared to meet its cost. The growing emphasis on healthy aging, with its resulting expansion of lifespans, will make these imperatives more important than ever to achieve.5
The reason most people do not plan early enough for LTC is that, since its establishment in 1965, Medicaid has paid for most expensive formal LTC not only for the poor but also for the middle class and many affluent people. The fallacy of impoverishment—the mistaken belief that eligibility for Medicaid’s LTC benefits requires spend down of income and assets into destitution—has prevented analysts from seeing this connection between Medicaid’s availability and the public’s seemingly irrational denial of LTC risk. The problem is not that people intentionally plan to use Medicaid if they ever need LTC. Few know who pays for LTC, and most wrongly believe Medicare does.6 Rather, Medicaid’s actual availability when care is needed (usually many years later) enables consumers’ denial of the risk and cost and leaves them unprepared and unprotected when confronted with chronic long-term illness.
Thus, the fundamental solution to the LTC policy problem is to direct the public’s attention to this large risk and cost earlier—before it is too late for them to prepare personally. That has been a major goal of LTC public policy ever since Medicaid’s LTC expenditures spiked far above original expectations in the 1970s. Through the 1980s and 1990s and into the mid-2000s, policymakers of both political parties sought to ensure that escalating Medicaid LTC expenditures went only to the people who needed them most. Numerous laws attempted to discourage the overuse of Medicaid LTC benefits by people who could and should pay for their own care. Those measures’ objective was to convince consumers that they should prepare for likely LTC costs in the future in order to avoid possibly devastating LTC expenditures that could consume their life savings. Although they were largely unsuccessful, the measures intended to scare the public straight point the way toward a better solution. But before designing and implementing a successful solution, it is crucial first to understand what policies failed and why they failed.
WHAT DID NOT WORK
Congress did not include LTC in Medicare but added nursing home coverage for the poor to Medicaid, recognizing its growing need and costs for an aging population. Medicaid expenditures exceeded expectations from the start of the program.7 LTC costs in Medicaid increased especially rapidly.8 Medicaid extended eligibility to anyone unable to afford nursing home care,9 and it reduced or eliminated strict eligibility criteria, transfer of assets restrictions, and mandatory liens that were previously commonplace in state welfare programs.10 This easy access to Medicaid nursing home care created a moral hazard that desensitized the public to LTC risk and cost.11 So long as LTC constituted a small risk of a catastrophic loss sometime in the distant future that a government program would then cover if necessary, most people ignored the risk. Most of those who later confronted catastrophic LTC costs ended up on Medicaid whether or not they knew from the beginning that Medicaid would pay.
Presidents and Congresses of both parties tried to subdue Medicaid LTC expenditure growth by suppressing the tendency to ignore LTC and rely on Medicaid in a long series of statutory and regulatory reforms. President Carter and a Democrat-controlled House and Senate took the initial step to rein in Medicaid LTC benefits in 1980 by imposing the program’s first ever limit on asset transfers to qualify for the program.12 That measure triggered the first law journal article on how to circumvent Medicaid eligibility rules and become eligible while preserving wealth.13
In 1982, President Reagan signed legislation passed by a Democratic House and a Republican Senate that lengthened and strengthened asset transfer restrictions and allowed states to impose liens to secure property for later recovery from recipients’ estates.14 In 1988, with Democrats controlling both houses of Congress, President Reagan signed legislation that, for the first time, required state Medicaid programs to penalize people who made inappropriate asset transfers.15 None of these measures succeeded in controlling LTC spending growth. Medicaid planning articles multiplied in formal legal publications and in the popular media. The techniques to qualify for Medicaid included hiding money, transferring assets, juggling resources, changing wills and titles to property, and setting up a Medicaid trust to access benefits without spending down savings.16
In the late 1980s, studies by the Office of the Inspector General (OIG) of the U.S. Department of Health and Human Services (HHS)17 and the Government Accountability Office (GAO)18 documented inconsistent state enforcement of the asset transfer, lien, and estate recovery regulations. The OIG report observed: “It is their children, after all, who stand to inherit whatever property remains after the costs of long-term care are paid and who currently reap the windfall of Medicaid subsidies. We must emphasize that the issue is enrichment of non-needy adult heirs, not denial of care to the elderly.”19 The government watchdogs recommended tightening Medicaid financial eligibility rules; making estate recoveries mandatory; and conducting further studies to analyze the relationships among Medicaid LTC eligibility, reduced private LTC spending, and low private LTC insurance take-up. A Democratcontrolled Congress concurred in 1993 when President Clinton signed legislation that required estate recoveries and made the asset transfer look-back period longer and stronger.20 But these efforts did little to reduce reliance on Medicaid LTC and nothing to abate an onslaught of legal treatises, law journal articles, popular books, magazine stories, and advertisements recommending “Medicaid estate planning.”21
In 1996, frustrated about continued abuses of Medicaid LTC, a Republican House and Senate sent President Clinton a bill that made it a crime to transfer assets for the purpose of qualifying for Medicaid.22 He signed what became known as the “Throw Granny in Jail Act.” When senior advocates objected, a Republican Congress replaced it in 1997 with the “Throw Granny’s Lawyer in Jail Law.”23 President Clinton signed this legislation, which made it a crime to accept a fee for advising a client to transfer assets to qualify for Medicaid, but the Justice Department deemed it unenforceable because transferring assets to qualify was no longer a crime in itself,24 and a federal judge later ruled the law unconstitutional.25
Nothing more was done to restrain Medicaid LTC overuse for almost a decade until a Republican Congress passed the Deficit Reduction Act (DRA), which President Bush signed in 2006. The DRA extended the asset transfer look-back period to a full five years. It also put the first ever cap on Medicaid’s home equity exemption, allowing states to set a limit from $500,000 up to a maximum of $750,000. The DRA’s home equity limit increased annually with inflation, reaching $688,000 and $1,033,000, respectively, in 2023. In 2018, the median home equity of homeowners ages 65 plus was only $143,500.26 Consequently, Hest, Alarcon, and Blewett “estimate that nearly the entire elderly population would meet the home equity threshold,”27 rendering it ineffectual to discourage Medicaid LTC eligibility except by the wealthiest.
When he signed the DRA, President Bush said, “The bill tightens the loopholes that allowed people to game the system by transferring assets to their children so they can qualify for Medicaid benefits. Along with Governors of both parties, we are sending a clear message: Medicaid will always provide help for those in need, but we will never tolerate waste, fraud, or abuse.”28
That was the expressed intent not only of the DRA but of the whole history of bipartisan legislation described above. Yet Medicaid LTC expenditures kept increasing despite this long, concerted effort. The public continued to ignore LTC risk and cost. Since 2006, no Congress has passed legislation to target Medicaid to those most in need. Nor has legislation advanced to encourage middle-class and affluent people to prepare early to be able to pay for their own LTC and avoid Medicaid dependency. Earlier economic recessions had led to legislation designed to spend Medicaid LTC money more wisely, discourage its use by the middle class, and encourage the non-needy to take personal responsibility. But after the Great Recession of December 2007 to June 2009 no further measures of that kind appeared.
WHAT HAPPENED AND WHY ACTION IS IMPERATIVE NOW
Innovative and risky new fiscal and monetary policies in effect since the 1990s explain why politicians permitted Medicaid spending to skyrocket over the past two decades. The Federal Reserve dropped interest rates to near zero. Public funds were spent with little constraint. The national debt soared, but few worried because servicing the debt at miniscule interest rates seemed manageable particularly given politicians’ generally short time horizons. With budgetary pressures relaxed, policymakers felt little incentive to address Medicaid’s excessive LTC spending or to reduce its long-standing moral hazard regarding LTC. But all that is changing today with higher inflation and interest rates and rising fiscal pressures from federal programs, particularly the massive unfunded liabilities of Social Security and Medicare. Budgetary pressures are again forcing policymakers to address Medicaid LTC financing expenditures.
CHANGING COURSE: FROM FAILED THREATS TO STRONGER INCENTIVES
Policies intended to scare consumers into planning privately for the risk and cost of LTC did not work. People could always ignore LTC and, if they needed expensive care over an extended period later, easily transfer the liability to Medicaid. The program’s financial eligibility rules allowed (1) ownership of practically unlimited exempt assets; (2) asset transfers five years in advance; (3) very large home equity protection; (4) major trust, annuity, and life estate exemptions; (5) large incomes so long as private health and LTC expenses were also high; and (6) substantial wealth transfer to heirs due to scant enforcement of the estate recovery mandate. Easy access to Medicaid meant the measures taken to encourage LTC planning and policies to encourage the purchase of private insurance for LTC largely failed. This condition will remain unless and until the public is engaged in LTC planning earlier in life.
HOW TO ENGAGE THE PUBLIC IN LONG-TERM CARE PLANNING WHILE THEY STILL HAVE TIME TO PREPARE
Step One: Eliminate Moral Hazard
Lawmakers should eliminate the moral hazard that has discouraged early LTC planning. That is, end the ability and practice to (1) ignore the LTC risk; (2) avoid the need to save, invest, or insure to prepare; (3) wait to see if expensive care is ever needed and, if it is; (4) transfer the liability to taxpayers by qualifying for Medicaid while preserving wealth. The methods people use to preserve wealth while qualifying for Medicaid LTC benefits late in life must cease. Those practices include but are not limited to:
- Purchase of exempt assets. This is the biggest, most costly, and hardest to measure method of artificial self-impoverishment to qualify for Medicaid. Medicaid requires that personal assets be spent down to a very low level (usually $2,000) before eligibility is granted. But the program does not require that such assets be expended for health or long-term care needs.29 This loophole allows Medicaid applicants to protect unlimited wealth by purchasing goods or services that are not included among countable resources. Such exempt items include an expensive home and—without any dollar limit—the following: one automobile, prepaid burial plans, one business including the capital and cash flow, term life insurance, household goods, personal belongings, and even individual retirement accounts (IRAs) in many cases.30 Medicaid planners routinely advise clients to maximize this path to eligibility. They provide long lists of exempt items for clients to purchase in order to reduce their countable wealth for Medicaid eligibility.31 No study has ever been conducted to measure this very easy Medicaid planning method’s incidence or cost.
Recommendation: Eliminate the exempt asset loophole by requiring that spend down of assets must be for health or LTC expenditures and documented in the case record as is already required and done for income spend down.32 - Home equity exemption. Current Medicaid law exempts between $688,000 and $1,033,000 of home equity, depending on the state. As home equity is most seniors’ biggest asset, protecting this wealth from LTC liability discourages responsible and early LTC planning. Financial tools and methods such as reverse mortgages and home equity loans enable individuals and families to access otherwise illiquid home equity for the purpose of funding private home-based LTC. As the legitimate purpose of Medicaid is to ensure access to quality LTC for the underprivileged, the program should not shelter home equity from eligibility consideration on behalf of middle-class and affluent applicants. Otherwise, Medicaid operates as free inheritance insurance for heirs instead of a safety net for those in need.
Recommendation: Eliminate the Medicaid home equity exemption according to a phase-in schedule with enough advance warning to incentivize early LTC planning without unduly affecting people already too old to prepare. - Medicaid Asset Protection Trusts (MAPT). “A Medicaid Asset Protection Trust is exactly as it sounds—a trust designed to protect assets from being counted for Medicaid eligibility.”33 Putting wealth, including real property, into an MAPT five years ahead of application for Medicaid LTC benefits removes unlimited amounts from eligibility consideration or spend down requirements.
Recommendation: Prohibit MAPTs immediately for all applicants and recipients. Once the law is changed, Medicaid legal advisers will self-enforce by no longer using or recommending the practice. - Medicaid Compliant Annuities. “A Medicaid Compliant Annuity is a single premium immediate annuity (SPIA) that contains zero cash value and provides income to the owner. Properly structured, this annuity functions as a spend-down tool that eliminates excess countable assets, allowing the nursing home resident to become eligible for Medicaid benefits.”34 There is no limit on how much wealth can be sheltered with a Medicaid compliant annuity. A congressional study cited a Rhode Island resident sheltering $400,000 and a Virginia resident sheltering $900,000 this way.35
Recommendation: Eliminate Medicaid-compliant annuities as a means to qualify for Medicaid while preserving wealth at any age. - Five-year asset transfer look-back. Assets transferred for the purpose of qualifying for Medicaid within five years of application are used to determine eligibility according to a formula that delays eligibility based on the amount of the transfer.36 Assets transferred more than five years before application are not considered no matter how great the amount divested. Because the median period of time from diagnosis to death in dementia cases is five years,37 families that transfer assets at early signs of mental weakening can entirely avoid Medicaid spend down requirements. Because real property ownership and transfers are publicly recorded, easy to check, and represent the largest portion of seniors’ wealth, the look-back period to discourage their transfer for purposes of Medicaid qualification should be much longer. It is unlikely that so many people would become Medicaid eligible and join the most expensive dually eligible recipients of Medicaid and Medicare if they were under notice of asset transfer limits 20 years in advance instead of five.
Recommendation: Expand the Medicaid asset transfer look-back period from five to 20 years. As all real property transfers are recorded and often automated now, checking for a look-back of 20 years is no more difficult than the current five-year look-back requirement. People would be much less likely to initiate asset transfers to qualify 20 years ahead of a potential LTC need as they routinely do five years ahead. In other words, this rule would be self-enforcing and not generally require enforcement 20 years later at the point of Medicaid application.
A systematic review of Medicaid income and asset eligibility loopholes (described and promoted in the vast formal legal literature on Medicaid estate planning38) would reveal many more oversights in Medicaid law and regulations that discourage responsible LTC planning and smooth the way onto Medicaid for people who do not plan for LTC. Some of the more egregious examples include spousal refusal, life estates, and half-a-loaf strategies.39 These should be eliminated as well. At a minimum, the GAO should immediately undertake a systematic study of Medicaid LTC eligibility rules and enforcement to ascertain the incidence and costs of these major loopholes. GAO should examine a valid random sample of Medicaid LTC cases generalizable to the national universe of such cases. Such a study should employ more intense review and verification techniques than are used by state Medicaid agencies. Severe staff and financial shortages cause the state agencies to miss applicants’ unreported income and resources, resulting in eligibility errors that closer scrutiny would reveal. Establishing national LTC financial eligibility error rates would finally reveal how much Medicaid loses as a safety net for the needy and how large its moral hazard impact is on the non-needy due to eligibility loopholes and errors.
How These Policy Changes Would Impact the LTC Market
Without any government program ensuring both the financing of LTC benefits and asset protection in the future, consumers would be far more concerned about LTC risk and therefore much more likely than they are now to save, invest, or insure against the risk. Fewer middle-class and affluent people would end up dependent on public assistance, so the public safety net could do a better job for the truly needy. Adult children would encourage and assist their parents to plan ahead instead of turning to Medicaid for relief when needed. Principles of personal responsibility guided by risk management techniques would prevail. More private financing would flow through the service delivery system relieving LTC providers from the burden of notoriously low Medicaid reimbursement rates. The market would set prices and allocate resources to meet consumer preferences instead of providers offering only what the government is able and willing to finance. Home- and community-based services would dominate—because that is what people prefer—and investors, entrepreneurs, and companies would be rewarded for providing these services. Nursing homes would still have an important role, but they would primarily provide skilled sub-acute and rehabilitative care rather than long-term custodial assistance.
These policy changes should be phased in so that they affect older people less or not at all and give younger people enough time to adapt. For example, people 55 or older and younger people with chronic disability or early onset dementia could be exempted from the change altogether. Current rules would remain in effect for them as they age into their 80s, the time of life when LTC becomes most likely. People 45-54, newly on notice that they can no longer count on easy access to Medicaid LTC while preserving wealth, should be expected to have a minimal level of LTC savings, investment, or insurance in place by age 65 sufficient to offset their average LTC liability. Likewise, people younger than 44 should be on notice that they need to have sufficient resources set aside by age 65 to offset their average catastrophic LTC risk. How each of these age groups can reasonably be expected to achieve these levels of protection is addressed below under Steps Three and Four.
We will need to monitor and enforce compliance with these new expectations regarding LTC planning. Without either, we can expect widespread non-compliance, leaving many unprotected for LTC risk as now but no longer protected against asset spend down in the future as before. Private fiduciary organizations could be tasked with identifying individuals’ LTC risks and to follow up with each person until the risk is covered. There could be a role for some level of government to follow up with people who remain derelict in this responsibility. Artificial intelligence could help monitor and administer a program to incentivize early LTC planning.40
Step Two: Publicize LTC Risk and Cost
Once Medicaid is preserved for the truly needy by preventing people from using it late in life and protecting their wealth, that change should be publicized widely. Without the ability to access government programs to finance LTC later in life while preserving wealth, people will have far greater incentives to engage in proper planning. From Washington State’s experiment in payroll-funded social insurance for LTC, we know that individuals will prepare once they are confronted with the urgent need to deal with LTC risk.
Washington Governor Jay Inslee signed a law in 2019 establishing the WA Cares Fund. The program was designed to charge workers a 0.58 percent payroll tax beginning January 1, 2022, to fund a lifetime LTC benefit of up to $36,500 after a 10-year vesting period. It faced strong public opposition, failing twice to receive citizens’ support at the ballot box.41 To make WA Cares more attractive to voters, an opt-out choice was added that allowed people to avoid the payroll tax by owning private LTC insurance purchased no later than November 1, 2021. As of August 15, 2022, 475,072 Washingtonians had taken that option,42 overwhelming the private LTC insurance carriers’ ability and desire to supply the product.43 Carriers, backlogged by the heavy new demand, worried the new policies taken out in minimal amounts to avoid the payroll tax would quickly lapse, creating an administrative headache and expense.
The key insight of the WA Cares Fund experience is that it took forcing people to pay immediately for LTC to get them to purchase private insurance for the risk. Prior to the Washington experience, no amount of scaring people about LTC cost or encouraging them with tax incentives persuaded many to buy the product. After WA Cares offered a way to opt out of its payroll tax, LTC insurance sales exploded. Nationally, more than three times as many people purchased the product in 2021 compared to 2020. Most of these new buyers were Washingtonians seeking to escape the WA Cares program’s payroll tax.44 Adding the opt out harmed the program by diverting individuals with higher incomes and more favorable LTC risks to private coverage, but it also pointed the way to better LTC policy.
Clearly, an important answer to the LTC challenge lies in making LTC risk and cost real for consumers earlier in their lives. Eliminating Medicaid eligibility loopholes would create this condition, and it does so without threatening all workers with a new, economically harmful payroll tax as in the WA Cares example. Publicizing the change in future Medicaid LTC eligibility across the country, at least as widely and frequently as WA Cares was promoted to Washingtonians, should result in a similar increase in consumer demand for any and all private means to save, invest, or insure against LTC risk and cost.
Step Three: Reconceptualize the LTC Challenge
LTC risk and cost are both frightening and seemingly so distant in the future that most people choose to ignore them, especially in the face of more immediately pressing responsibilities. One key to refocus consumers on LTC is to reconceptualize the problem, with new information that reveals it is less intimidating than usually conceived. In the past several years, new research has suggested that LTC may not be such an overwhelming financial risk for most people as previously assumed.
In 2022, HHS’s Assistant Secretary for Planning and Evaluation estimated “that over half (56%) of Americans turning 65 today will develop a disability serious enough to require LTSS.”45 But that means nearly half, 44 percent, can expect to have zero LTC need. In fact, “While individuals on average will need 0.8 years of paid LTSS, 55% of older adults will not use any paid LTSS.”46 Furthermore, on average “an American turning 65 today will incur $120,900 in future LTSS costs, measured in today’s dollars.”47 This amount could be financed by setting aside48 the present discounted value of $69,80049 at age 65.50 Earmarking $70,000 at age 65 for future LTC expenses does not sound nearly as daunting as insuring against the full catastrophic LTC risk potential of $250,000.51 If people begin LTC planning earlier than age 65, even less would be needed to set aside.52 In essence, the burden is much more manageable than previously conceived.
Once the principle is established that every person has a responsibility to cover an objectively determined amount of LTC liability by a certain age, each person’s target amount could be adjusted in a way that treats people fairly based on their sex, income, health status, and other relevant demographic characteristics.
People Already Have More Funds Available for LTC Than They Are Using Now
There is more good news. In June 2019, Johnson and Wang “simulated the financial burden of paid home care for a nationally representative sample of non-Medicaid community-dwelling adults ages sixty-five and older.”53 They “found that 74 percent could fund at least two years of a moderate amount of paid home care if they liquidated all of their assets, and 58 percent could fund at least two years of an extensive amount of paid home care.”54 Furthermore: “Nearly nine in ten older adults have enough resources, including income and wealth, to cover assisted living expenses for two years.”55 So the potential LTC financial burden is much more manageable than we thought. The evidence that people accumulate substantial savings that could be used for LTC if they had more incentive to do so is very encouraging. Assuming the removal of Medicaid’s generous financial eligibility rules that obviate the need to plan for LTC, the path forward will be much less fraught.
Exactly How Much Wealth Do People Have and Why Aren’t They Using More of It for LTC?
This paper’s Appendix answers those questions based on new research and draws the appropriate conclusions for LTC financing policy reform.
Step Four: Show Younger People a Better Way
Even if the LTC financing challenge is not as daunting as previously believed and families possess more wealth than we thought, we still need ways to make it easier for younger people and families to identify and put to use the means at their disposal to prepare for LTC risk and cost. Government should advise all Americans by age 25 that LTC planning is a personal responsibility planning for which should start no later than age 40 and be achieved by age 65.
The termination of all methods to qualify for Medicaid LTC benefits late in life while preserving wealth should be disclosed, publicized, and frequently reiterated in state and federal government publications. By age 65, most Americans should be prepared to pay for their expected LTC expenses, which would require them on average to have $70,000 saved, set aside, or insured for that purpose. LTC Choices 1-7 below suggest some methods by which people could fulfill their LTC planning responsibility. Entrepreneurs can be expected to produce many more.
A private fiduciary organization similar to Underwriters Laboratories could counsel Americans on LTC risk and cost, propose methods to prepare, evaluate their proposals to meet their responsibility, and help them achieve the needed protection. Private insurers could estimate individual need and recommend the necessary level of coverage with quality control review by independent actuaries or auditors. Following are several possibilities that could satisfy the need to plan for LTC with minimal financial disruption for individuals and families carrying other financial responsibilities at the same time. The basic strategy is twofold: (1) to aim LTC planning toward a more realistic goal of meeting each individual’s probable risk and (2) to minimize the immediate cost of preparing for LTC risk by earmarking funds already accumulated in retirement savings to be used for LTC if and only if LTC becomes necessary
Methods to Satisfy Individual LTC Responsibility
LTC Choice #1: Private Insurance. Purchase private LTC insurance that meets minimal coverage standards based on age, sex, health status, etc. Instead of huge premiums to cover potential lifetime coverage of expensive nursing home custodial care,56 adequate insurance coverage for each individual’s personal risk will prove much more affordable. Most analysts believe private LTC insurance is unlikely ever to penetrate enough middle-income households to become a significant payment source. But they have always assumed that people would need much more coverage at too great a cost to attract enough buyers to make a big difference. That assumption may be wrong.
Smaller, less expensive LTC insurance policies could have a disproportionately large impact on the aging public’s ability to afford senior housing, including home care and assisted living. The National Investment Center reported that reducing the annual cost of senior housing by $15,000, from $60,000 to $45,000 per year, would expand the middle market for senior housing57 by 3.6 million individuals, enabling 71 percent of middle-income seniors to afford the product.58 Where could consumers find that extra $15,000 to bring the cost of senior housing into reach? The premium for an annual LTC insurance benefit of $15,000 would only cost a small fraction of the premium required for the comprehensive coverage that consumers find so financially daunting now. Unfortunately, insurance regulations sometimes forbid carriers from offering coverage with a benefit of less than $18,000 per year. Once again, well-intentioned regulation stands in the way of sensible LTC policy and planning.
LTC Choice #2: Investment Accounts. Establish a new tax-deferred investment account similar to the 401(k) or IRAs already available to cover future predictable LTC expenses. Consider a fully tax-exempt investment account as an even greater savings facilitator. To soften the impact of contributing to an extra retirement account, savers could be allowed to use a portion of their existing retirement accounts or health savings accounts to satisfy the LTC responsibility.59 The strategy is to use a portion of funds already saved for other purposes by allocating them for LTC if and only if LTC becomes necessary.
LTC Choice #3: Retirement Savings. Allow a portion of retirement savings to meet the LTC planning responsibility. At the end of March 2023, total U.S. retirement assets were $35.4 trillion, including $12.5 trillion in IRAs, $9.8 trillion in defined contribution accounts, and $10.9 trillion in combined government and private defined benefit plans. Annuity reserves outside of retirement accounts add another $2.2 trillion.60
LTC Choice #4: Home Equity. Over 78 percent of age 65 and over households own homes.61 Many could lien their home equity to support LTC or withdraw sufficient funds through reverse mortgages to purchase private LTC insurance as in LTC Choice #1. The $12.4 trillion in home equity held by people 62 years of age and older62 would both cover the LTC expenses for a large portion of them and send huge waves of desperately needed private revenue into the LTC service delivery system. This new private revenue—at rates 50 percent more than what Medicaid pays—would improve care quality and access for all LTC patients, including those dependent on public financing. Estimating potential savings to Medicaid from this source is difficult. Little is known about current home ownership by Medicaid LTC recipients, because Medicaid exempts most home equity. A dated (but unique) 1989 GAO study found, “About 14 percent of the Medicaid nursing home residents in the eight states GAO reviewed owned a home,” and “By using home equity to defray Medicaid costs as Oregon does, the six states that now lack recovery programs could recover about $85 million [$218 million in today’s dollars] from recipients admitted to nursing homes.”63 Diverting home equity earlier in life to finance LTC risk later, instead of relying on Medicaid and then attempting to recover from estates after death, would unleash the huge potential of home equity to finance quality LTC for more people.
LTC Choice #5: Life Insurance. Many life insurance policy holders can carve out enough of their cash values or death benefits to meet their personal LTC responsibility. Total life insurance coverage in the United States was $21.2 trillion by the end of 2021.64 There are several ways to access the cash value of life insurance without dying. They include dropping the policy to collect its surrender value, selling the policy by means of a “life settlement,” and withdrawing funds or borrowing from the policy.65 Even a term life policy, with no cash value, can sometimes be sold.66 The current perverse incentive created by government policy when people need LTC is to liquidate cash value life insurance, spend the money on exempt assets, and then apply for Medicaid when the funds are gone. Eliminating that loophole would free up trillions of private life insurance value to offset public LTC expenditures.
LTC Choice #6: The Deferred Reverse Estate Annuity Mortgage (DREAM). This option—a legally binding and officially recorded lien on one’s estate set aside for LTC—does not currently exist, but it is similar to the existing Medicaid estate recovery obligation except that it moves the responsibility forward in time and ensures eventual LTC funding availability. The DREAM mortgage satisfies the LTC planning responsibility only if it is formally executed, is legally recorded, and applies to all property that will pass inside or outside of a probated estate. Unlike asset transfer limitations and estate recovery, this option secures the property so that it is available to pay for care in the private market. This is a way for people to prepare for LTC risk and cost, lock in the ability to pay privately for care, and have no immediate need to expend income. They merely obligate a portion of their estates for their LTC if needed. Any remainder would pass to heirs, although it would be unprotected by Medicaid, as it is currently. This is the easiest and least intrusive of all the methods to satisfy the LTC planning responsibility.
LTC Choice #7: Capture the other end of the age spectrum from estates. People who begin saving, insuring, or setting aside resources for LTC before age 40 could receive a reduced LTC responsibility level. So, in addition to the lower discounted present value of their LTC responsibility, they would have an added incentive to begin LTC planning earlier. Employers could introduce LTC responsibility to job seekers in their early 20s. Increasingly, younger people are having to care for their parents and grandparents. If they become sensitized to the need for LTC planning earlier than others and they take action, their LTC responsibility could be satisfied earlier and at less personal cost than for others who begin preparation later in life.
All seven of these options are manageable by private companies—such as employers, insurers, banks, or brokers—eliminating much of the huge federal and state bureaucracy currently managing Medicaid LTC eligibility determination and estate recovery. Other tools and methods of satisfying the LTC planning objective will evolve naturally in a market not distorted by Medicaid rules that reward failure to plan.
Poverty Reconceptualized:
Clearly there is enough wealth in the American economy to fund quality LTC for all Americans if it is mobilized with better incentives than prevail now. In fact, poverty, properly measured, is already uncommon in the United States.67 A 2018 Cato Institute study reports, “Improved estimates of poverty show that only about 2 percent of today’s population lives in poverty, well below the 11 percent to 15 percent that has been reported during the past five decades.”68 How can that be? “By design, the official estimates of income inequality and poverty omit significant government transfer payments to low-income households; they also ignore taxes paid by households.”69 What is the bottom line? “The net effect is that pretax data overstate the true income of upper-income households by as much as 50 percent, and missing transfers understate the true income of lower-income households by a factor of two or more.”70 The rich are poorer and the poor, richer than we thought. “More than 50 years after the United States declared the War on Poverty, poverty is almost entirely gone.… Public policy debate should begin with the realization that only about 2 percent of the population—not 13.5 percent—live in poverty.”71
The official poverty level calculated by the government does not involve the level of total destitution some may associate with it. Consider a poor household’s consumption a decade ago according to a Heritage Foundation analysis:
The typical poor household, as defined by the government, has a car and air conditioning, two color televisions, cable or satellite TV, a DVD player, and a VCR. By its own report, the typical poor family was not hungry, was able to obtain medical care when needed. The typical average poor American has more living space in his home than the average (non-poor) European has.72
Worries about income inequality are also misplaced. “By not counting two-thirds of all transfer payments as income to the recipients of the transfers and not counting taxes paid as income lost to taxpayers, government statistics dramatically overstate income inequality.… The facts reveal a very different and better America than the one currently described in debates across much of the political spectrum.”73 Phil Gramm and John Early concluded: “By eroding self-reliance, worker pride and labor-force participation, government-generated income equality undermines the very foundations of American prosperity.”74
Applying this corrected understanding of poverty and “inequality” to the challenge of financing LTC suggests, as do other facts referenced above, that America has more sources of wealth to work with than previously contemplated by most experts. Mustered and employed more sensibly, these resources would suffice to ensure access to quality LTC for all Americans.
Managing the Back End
This proposed approach of withdrawing Medicaid asset protection in the future and encouraging private LTC planning in the present will not cover everyone who may need LTC later. Some will be unable to fund any of the options that will become available. Others will decide not to plan. But most people, faced with an immediate requirement to confront LTC risk and cost, will likely take steps to prepare. Still, 14.7 percent of people turning 65 will incur LTC expenses of $250,000 or more, nearly half of which Medicaid already pays.75 Much relieved of the need to cover most of the cost of LTC, Medicaid could continue as the payer of last resort for these people.
With the techniques used to qualify for Medicaid while preserving wealth eliminated in the future for people currently under age 55, over time Medicaid LTC benefits will no longer be available to people while also allowing them to retain income and resources. Far fewer people will be dependent on Medicaid. At that point the program should pay full private market rates so remaining recipients can receive high-quality home care, assisted living, or nursing home care as needed. The existing two-tier LTC service delivery system—in which Medicaid recipients receive lower cost, less desirable care compared to market-rate private payers—should largely end. Resources accumulated in private hands through insurance, targeted savings or from reverse mortgages or liens, will suffice to fund the vast majority of all LTC for most people. In fact, even before those measures are employed, most older adults could already finance substantial LTC if required to use resources they already own for that purpose.76
With most LTC provided within the private market at market payment rates, LTC providers would prosper instead of being underpaid by Medicaid as they now are. Private market competition would ensure adequate compensation for LTC nursing and support staff, which would eliminate their shortage. In addition, fewer people would need to provide direct care themselves for friends and family. They could instead provide love and support without having to provide bathing assistance or change adult diapers. Entrepreneurs would compete to find newer and better service delivery methods. The financial burden on government and taxpayers would lessen substantially. Impoverishment due to LTC, to whatever heretofore unsubstantiated level it has existed,77 would mostly disappear.
Why Not Social Insurance Instead?
Why not simply require by government fiat that everyone must pay a tax so that all can receive a LTC benefit when it is needed? That is the sirens’ song of social insurance.
Why is social insurance so appealing to intellectuals and politicians despite their inability to get such plans approved by voters? By compelling citizens to participate in the scheme, social insurance avoids the biggest problem of voluntary private insurance. People are not forced to purchase private LTC insurance, so many do not, leaving too many unprotected. By forcing everyone to pay for social insurance, government ensures that the substantial financial risk of LTC is spread across the whole population. Social insurance avoids adverse selection, the problem of only those most likely to use the insured benefit purchasing private insurance for it, resulting in a solvency death spiral. Despite these apparent benefits, proposals for compulsory LTC social insurance have never achieved the approval of voters and taxpayers. Why?
The compulsion and universality of social insurance also have vital downsides, including loss of freedom and some perverse incentives. Because social insurance spreads (but does not price) risk, it rewards irresponsibility and punishes responsible behavior. Private insurance, on the other hand, spreads but also prices risk. People pay more for private life insurance if they smoke, so it discourages smoking and rewards healthier behavior. Social insurance does the opposite. It charges everyone the same regardless of how much risk they bring into the risk pool, thus rewarding high-risk people and behaviors while punishing low-risk people and behaviors. Private insurance rewards personal responsibility and self-reliance, whereas social insurance rewards and thus encourages government dependency.
The moral precept of social insurance is “from each according to his ability, to each according to his need,” the fundamental principle of socialism. Across a society the incentives and disincentives of social insurance undermine personal responsibility, discourage individual effort, and lead to excessive reliance on others for support, including government authorities exercising their monopoly of the legitimate use of force. Social insurance always and everywhere tends toward collective mediocrity and individual failure. In light of the short-term solvency denouement of Social Security and Medicare, we should view new social insurance plans with increasing skepticism.
SUMMARY AND CONCLUSION
Albert Einstein said, “We can’t solve problems by using the same kind of thinking we used when we created them.”78 The kind of thinking that created LTC’s problems is that markets cannot provide the services people need without massive government regulation and financing. No other way of thinking about the problem has been seriously considered. But recent research suggests how to reconceptualize the quandary policymakers face so that LTC is not such a titanic crisis and may be fixable with a market-based solution.
Eliminating the means by which people have ignored LTC planning early in life while preserving wealth and qualifying for Medicaid later can encourage consumers to prepare early and responsibly for future LTC risk. Showing them ways to set aside wealth that they already possess or will accumulate over time can enable them to manage the LTC risk while fulfilling other responsibilities such as raising a family, car and house payments, retirement, and education savings.
LTC need not be the overwhelming challenge that pushes analysts toward “easy” solutions involving economically harmful payroll taxes, government compulsion, and public entitlement programs. Properly conceived and with the right financial tools and incentives available, LTC can be fully financed and vastly improved without undue pressure on families, consumers, or taxpayers.
APPENDIX: EXACTLY HOW MUCH WEALTH DO PEOPLE HAVE AND WHY AREN’T THEY USING MORE OF IT FOR LTC?
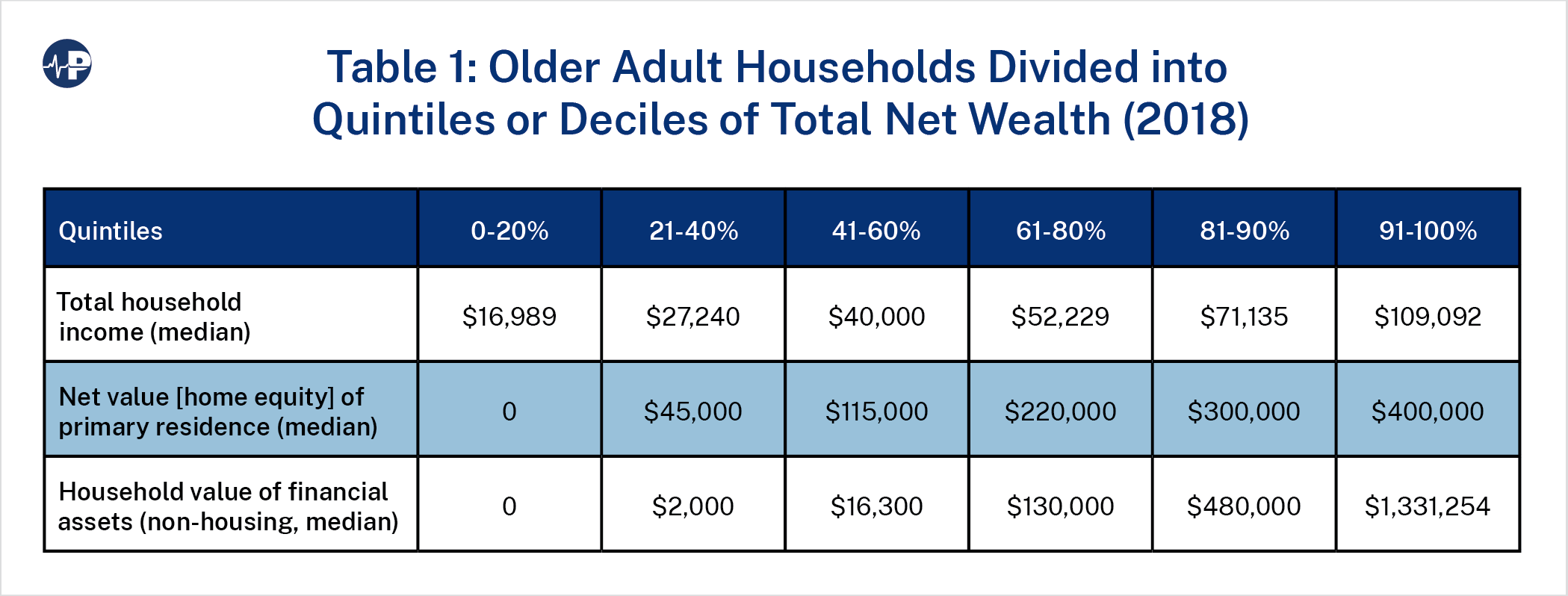
The table above is condensed from a more detailed version published by the National Council on Aging and the LTSS Center in a February 2023 report. It displays the wealth of older adult households by quintile through 80 percent and then by decile to 100 percent. The report states that “the bottom 20%, approximately 11 million households, have no assets. This group has a 2018 median income of $16,989 and would be unable to rely on personal finances to pay for LTSS, especially with rising costs of care.”79 Clearly, this is an economic group for which Medicaid LTC benefits are intended to provide a safety net.
The report continues: “The next three quintiles (21–40%, 41–60%, and 61–80%) of older adults saw modest increases in their financial assets between 2016 and 2018, but these individuals would still be unable to afford more than two years of nursing home care in a semi-private room or four years in an assisted living community if their median income and household value of financial assets were added together. Despite adults’ preference to age in place, 60% of adults would be unable to afford two years of in-home long-term services and supports.”80
That conclusion is striking. If 60 percent of middle-class aging Americans cannot afford two years of in-home LTSS, then it follows that 40 percent can. If so, that would cover the average LTC risk and cost for most of them: “[O]ver half of adults 65 and older will need LTSS for less than two years … .”81
But are people actually spending down their wealth for LTC? How much of their income, “household value,” and other financial assets do people actually use to fund their own LTC? Conventional wisdom holds that high LTC costs force wide swaths of American elders into impoverishment, leaving them dependent eventually on Medicaid. Is that what happens? Do middle-income people have any other choice? If faced with high LTC costs, would people in the fourth wealth quintile (61-80 percent) need to spend down their wealth before qualifying for Medicaid-financed LTC?
Their median total household income is $52,229. The rule of thumb for income is that anything below the cost of a nursing home is not disqualifying. That is because private health and LTC expenditures are usually deducted from income before comparing the balance to Medicaid’s very low allowable limit.82 A well spouse would keep any income in his/her sole name plus a “monthly maintenance needs allowance” of up to $2,465 or $29,580 per year (as of 2023) from the recipient’s income. Any remaining income in the Medicaid recipient’s name would go to offset the program’s cost for his/her care, but if there is an estate recovery later, the recipient would be liable only for what Medicaid spent for his/her care, which is much less than what the private pay cost would have been.
Thus, while some private income goes for care, this out-of-pocket cost—mostly Social Security income (explained below)—merely reduces Medicaid’s share of the extremely low reimbursement, often less than the cost of care, that the LTC provider receives. Although the recipient is paying out of pocket, he/she is not commanding the better access and higher quality care associated with paying privately. He/she is trapped in the lower Medicaid level of America’s two-tier LTC system.
What about assets? Must they be spent down before getting Medicaid? The “net value of primary residence” (i.e. home equity) of people in the fourth wealth quintile is $220,000. Does that amount interfere with Medicaid LTC eligibility compelling asset spend down? No. Medicaid exempts a minimum of $688,000 of home equity and up to $1,033,000 in some states. Even the richest people would qualify for Medicaid based on their home equity of $400,000.
But, as is widely known, Medicaid allows applicants/recipients to hold no more than $2,000 in “countable” assets while qualifying for or receiving Medicaid LTC benefits. The fourth quintile’s “household value of financial assets (non-housing, median)” is $130,000. But that is just a starting point. If there is a spouse, Medicaid computes the couple’s jointly owned assets and sets aside half—not to exceed $148,620 but never less than $29,724 (as of 2023)—for the “community spouse.” Then Medicaid takes out the non-countable assets people own, such as “pre-paid burial and funeral expenses, an automobile, term life insurance, life insurance policies with a combined cash value limited to $1,500, household furnishings/appliances, and personal items, such as clothing and engagement/wedding rings.”83 Very few people in the fourth quintile of wealth will have much savings left after these deductions, but whatever remains can easily be converted to non-countable status by investing more money in the home or purchasing, in unlimited amounts, any of the other exempt items just listed.
When they confront high LTC costs, do middle-class people ignore these generous Medicaid financial eligibility limits and pay out of pocket? Do they voluntarily plunge themselves into real impoverishment from a sense of personal responsibility or shame at depending on public assistance? Some do. More used to. But nowadays information on how to qualify for Medicaid without spending down for care is universally available in magazine articles and self-help books, in legal treatises and on the internet. Google “Medicaid planning in [any state]” to find long lists of attorneys who specialize in qualifying clients for Medicaid while preserving their wealth. Even state Medicaid eligibility workers routinely explain to middle-class applicants how to speed up or entirely eliminate their “spend down” process by purchasing exempt assets. Workers report that people think of Medicaid (public assistance) as though it were an entitlement like Medicare.84 They ask, as Jane Bryant Quinn did in a 1989 Newsweek column, “Do Only the Suckers Pay?”85 So, no, ignoring easy access to Medicaid LTC benefits and paying out of pocket is the exception, not the rule.
But what about the conventional wisdom that people all across America must be, and actually are, spending down to impoverishment before obtaining Medicaid? If that is true, it should show up in the data. But it does not. The percentage of nursing home costs paid by Medicaid and Medicare has nearly doubled over the past half-century from 26.8 percent in 1970 to 52.3 percent in 2021, while out-of-pocket costs have shrunk by half in the same period from 49.2 percent in 1970 to 24.5 percent in 2021.86 Nursing home private-pay revenue has plummeted to 7 percent.87
The situation with home health care is very similar. America spent $125.2 billion on home health care in 2021, of which Medicare (37.2 percent) and Medicaid (34.2 percent) paid 71.4 percent. Private health insurance (not LTC insurance) paid 12.7 percent. Only 10.3 percent of home health care costs were paid out of pocket. The remainder came from several small public and private financing sources.88 Maybe people are spending down for assisted living. Some surely do, but “Almost 1 in 5 [assisted living] residents relies on Medicaid to pay for daily services (18%),” “61% of [assisted living facilities] are Medicaid certified,” and only “a small minority of state Medicaid programs do not cover services in assisted living.”89 Assisted living began exclusively as a private-pay option, but that is changing rapidly. Still, to count spend down for assisted living as an out-of-pocket LTC expenditure is dubious, because a large portion of the fee for assisted living covers room and board, not LTC.
So how can it still be that “Family out-of-pocket costs are also substantial, averaging $44,800 and accounting for 37% of the total” LTSS expenses, averaging $120,900 per person?90 The answer is another anomaly of Medicaid LTC financing policy: People receiving Medicaid LTC benefits are required to contribute all but a small portion of their income to offset Medicaid’s cost for their care. While this income “spend-through” is rarely considered, research from three decades ago documented that it is substantial, roughly half of what is reported as out-of-pocket costs.91 This matters because the spend-through income—mostly Social Security benefits, although correctly considered to be a private out-of-pocket expenditure for Medicaid LTC—is not asset spend down and does not come from people’s savings or home equity. Relatively little of what is reported as personal out-of-pocket LTC expenditures comes from savings or home equity expended for nursing home or home health care. Much of it is Social Security income that is vulnerable to that entitlement program’s potential insolvency and has been contributed by people already on Medicaid, some of whom are receiving Medicaid while residing in assisted living facilities or continuing care retirement communities (CCRCs).92 Removing private payments for assisted living and CCRCs, much of which cover room and board costs and not LTC, leaves much less reported out-of-pocket LTC costs remaining that could actually constitute consumption of life savings or real property assets.
Finally, analysts often refer to the University of Michigan Health and Retirement Study and its auxiliary, the Asset and Health Dynamics among the Oldest Old study for evidence to support their presumption that people are spending down assets to qualify for Medicaid LTC benefits. Research does show that people tend to decumulate assets rapidly at older ages, and many do qualify for Medicaid thereafter. But there is nothing in the data to link decumulation of wealth with spend down on health or LTC costs. Those sources show only that transitions to Medicaid eligibility occur. Such transitions may as likely be the result of Medicaid planning (i.e., artificial self-impoverishment) conducted many years before in anticipation of the future need for LTC.
The widespread belief that high LTC costs impoverish large numbers of aging Americans is unsupported by the evidence. Medicaid financial LTC eligibility rules do not exclude people up to and through the fourth quintile of wealth. Ample evidence suggests that the public is aware of methods to qualify easily for Medicaid LTC benefits or quickly learn how when expensive care costs arise. Private-pay revenue for LTC providers, including home health agencies and skilled nursing facilities, is low and falling. Private pay for assisted living and CCRCs—much of which does not go for LTC but rather for room and board—should not be bunched in with spending for home health and skilled nursing. In the absence of evidence of high out-of-pocket spend down for LTC, analysts should reassess what is actually happening and how to address reform.
In summary, middle-class Americans have enough wealth to fund their average expected LTC costs, and this wealth is largely exempt from Medicaid spend down rules. Information on how to access Medicaid LTC benefits without spending down is widely available, and there is no evidence of widespread LTC spend down resulting in impoverishment. So, one can conclude that changing Medicaid eligibility policy to remove the option to ignore LTC, shelter personal wealth, and rely on public benefits when LTC becomes necessary should free up enormous resources of private wealth to support LTC financing.