Reforming Government. Empowering Patients.
Navigation
Long-Term Care: The Problem


The Paper
This paper outlines the challenges and inefficiencies in the U.S. long-term care (LTC) system, emphasizing the heavy reliance on Medicaid and Medicare, the negative impact of government policies on private financing, and the urgent need for reform to improve care quality and financial sustainability.
Abstract
Providing and funding long-term care (LTC1) for the elderly is a large and growing challenge. Baby boomers start turning 85—the age at which health and LTC costs spike—in 2031, as Social Security and Medicare face insolvency. The government, mostly through Medicare and Medicaid, finances almost three-fourths of LTC expenditures (72.3 percent in 2020).2 Central planning, public funding, heavy regulation, and easy access to welfare benefits have caused most of LTC’s problems, such as nursing home bias, poor access and quality, inadequate revenue for care providers, caregiver shortages, and the terrible emotional and financial distress for caregiving families. Medicaid especially is responsible because, despite the conventional wisdom that it requires impoverishment, the program’s LTC benefits are routinely available not only to the poor but to the middle class and affluent as well.
The entrepreneurial private sector responded creatively to mitigate—though not completely resolve—the problems created by public financing and regulation. The dominance of Medicaid and Medicare financing for nursing homes and home care prevented alternative modes of LTC service delivery and financing from fully developing based on consumer preferences. Access to publicly financed LTC creates a moral hazard that discourages responsible LTC planning when people are still young, healthy, and affluent enough to save, invest, or insure for the risk. Policymakers should consider how public financing created and worsened LTC’s problems before proposing more of the same to address those problems. This paper outlines the problems caused by well-intentioned but ultimately damaging government LTC policies. A forthcoming paper will describe the best policy options moving forward.
The Problem
America’s LTC system is broken. It poorly serves, both financially and emotionally, the people who receive care as well as the workers and companies that provide care. Moreover, government funding and regulation are pervasive, whereas private financing and personal responsibility have declined substantially.
Leading LTC “reforms” to address this broken system have centered on expanding government programs. Examples include the Pepper Commission in 1990;3 the Commission on Long-Term Care, 2013;4 and the Biden administration’s “Build Back Better” plan.5 Based on analysis published in Health Affairs,6 two February 2016 reports by Leading Age,7 and the ad hoc LTC Financing Collaborative,8 many leading policy experts who support increased government involvement have coalesced around a consistent plan: compulsory, payroll-tax-funded social insurance to finance LTC. Having failed to achieve such a system nationally, analysts and advocates have moved recently to propose the same approach in several states, including Washington, California, Pennsylvania, and New York.9
Before adopting a new government program, policymakers should confront several questions: How did LTC become so dysfunctional in the first place? Would adding more government funding and control improve a delivery and financing system already dominated by both? Are there ways to address these problems that reduce dependence on government and engage consumers’ self-interest, personal responsibility, and individual effort more fully? What do policymakers need to know about the LTC market before they try to fix it with even more laws, regulations, and taxes? To answer those questions, understanding what services LTC includes, its history, and its financing is essential.
LTC Background
LTC includes a wide range of medical and social services that people require when they are unable to take care of themselves. LTC need may arise at any age due to injury, illness, frailty, or cognitive impairment, but the focus here is illness or frailty due to old age.
The probability of needing LTC is high. Seventy percent of people who reach age 65 will eventually develop severe need, and 48 percent will receive paid care.10
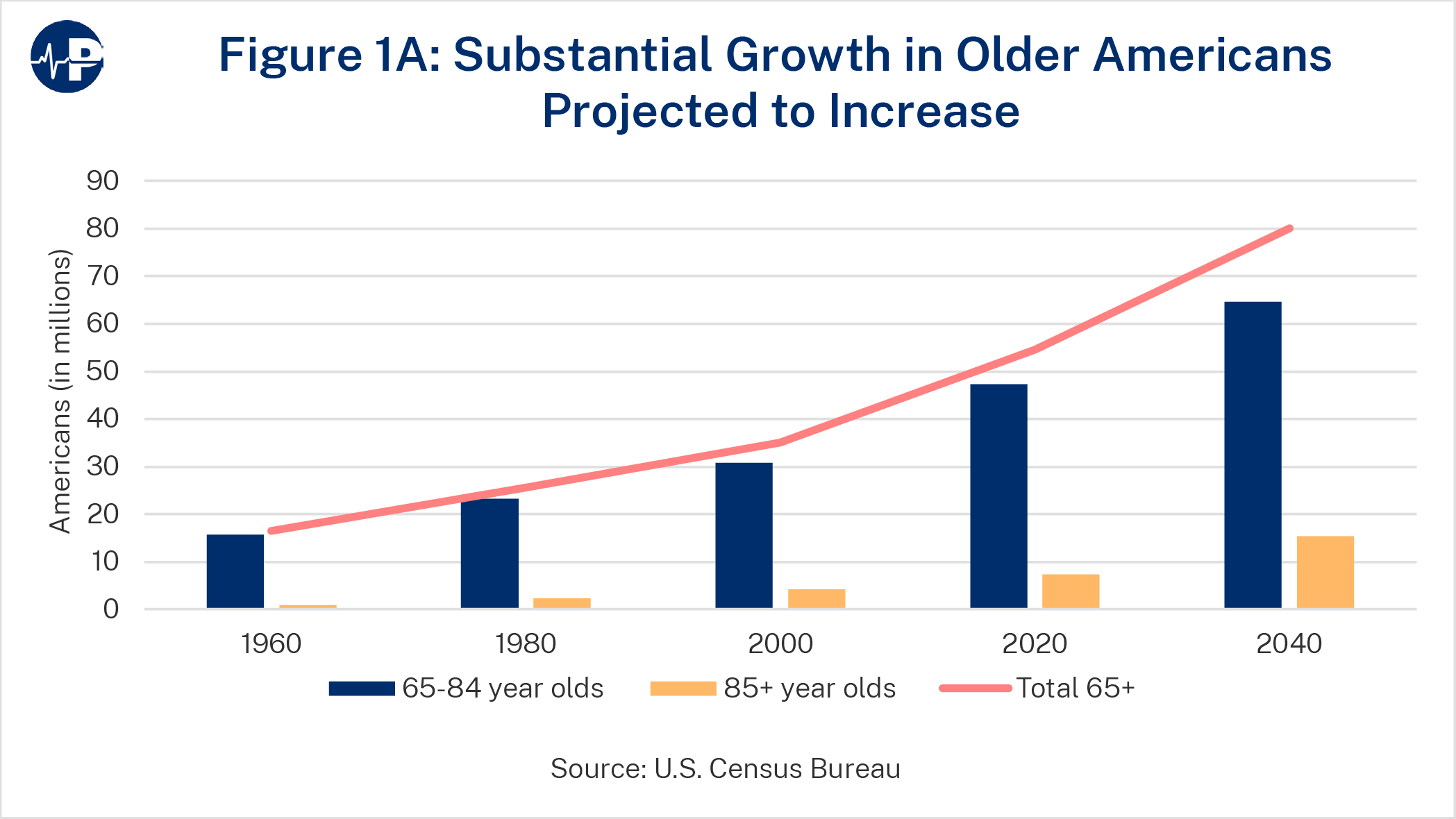
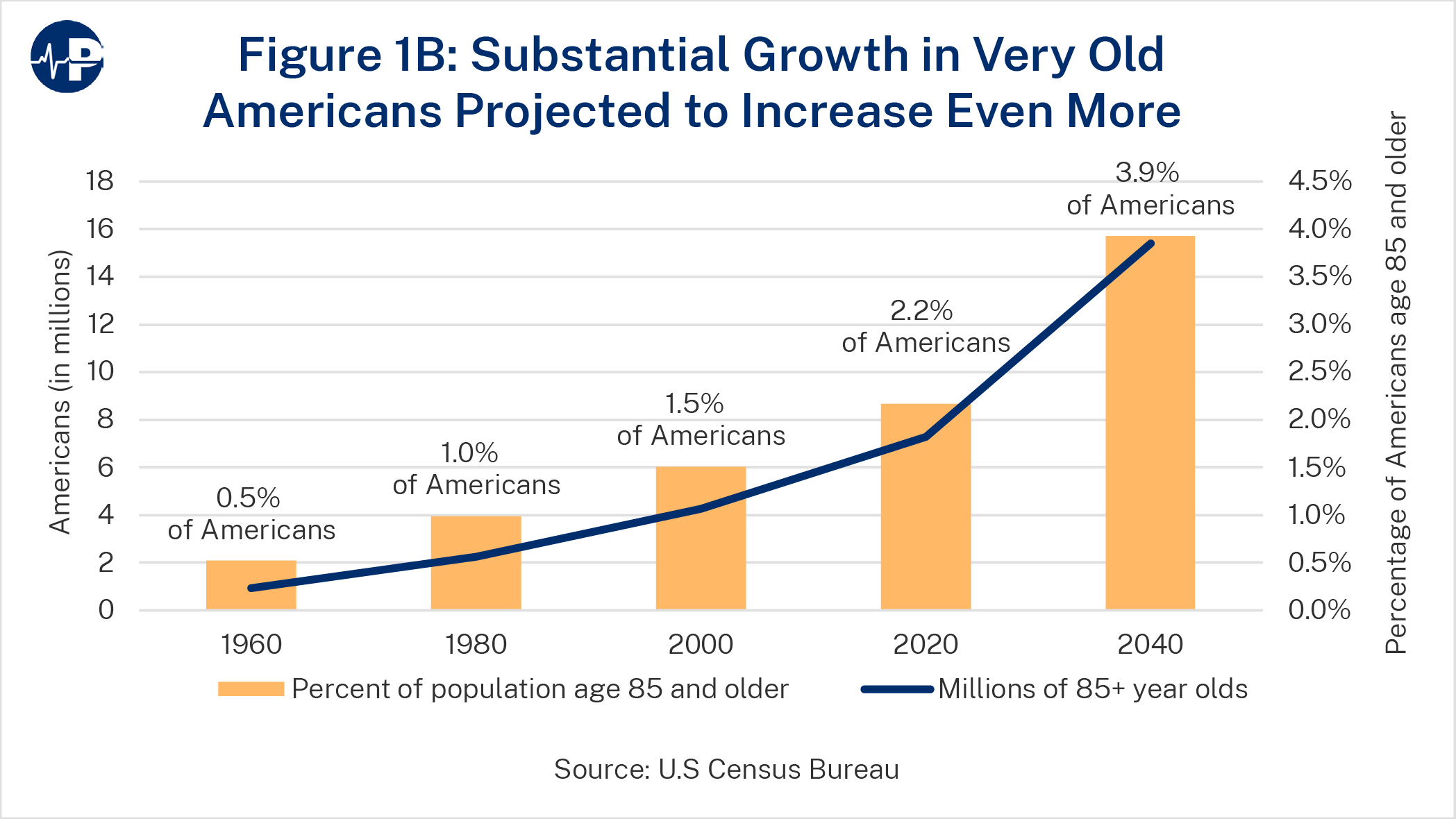
The need for paid care spikes around age 85.11 America’s 85 and older population is growing rapidly, as the following figure shows. Americans over the age of 85 are projected to be 3.9 percent of the population in 2040, substantially more than the 1.5 percent of the population they made up in 2000 and the 2.2 percent of the population they make up today. Americans over the age of 85 will continue to increase thereafter. The percentage will nearly triple between 2015 and 2050.12
Paid care is expensive, whether provided in a nursing home ($297 per day for a private room, $260 for a semi-private room) or assisted living facility ($4,500 per month) or at home by a home health aide ($27 per hour).13
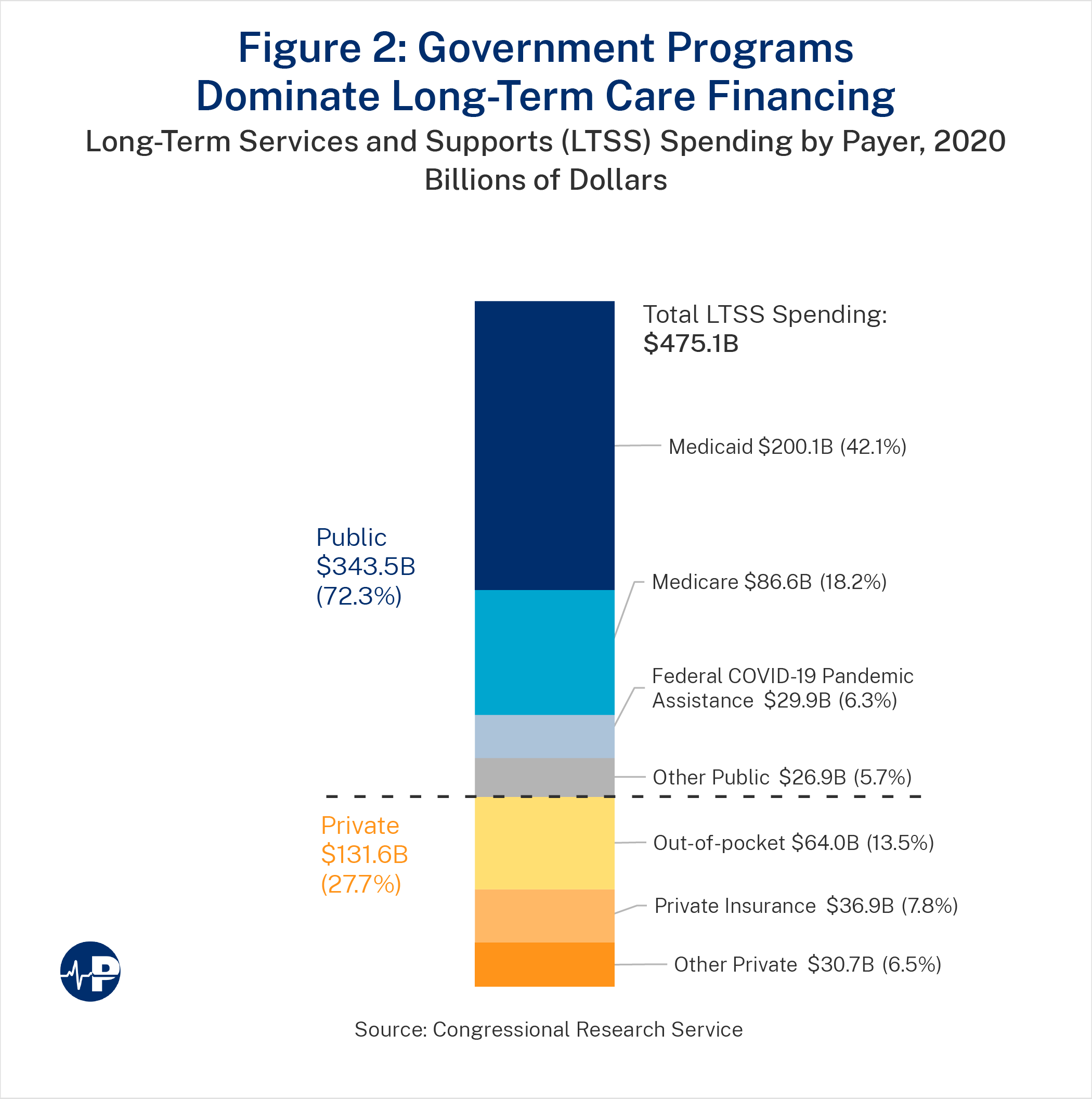
LTC spending in the United States was $475.1 billion in 2020,14 up 29.8 percent from $366.0 billion in 2016,15 with 72.3 percent coming from public sources—including 42.1 percent from Medicaid and 18.2 percent from Medicare—and 27.7 percent from private sources, including out-of-pocket expenditures (13.5 percent) and private insurance (7.8 percent).16 Besides this formal paid caregiving, families and friends provided unpaid care with an opportunity cost of $522 billion annually. To replace informal care with unskilled or skilled paid care would cost $221 billion and $642 billion, respectively.17
Medicaid’s and Medicare’s Role Financing LTC
Given the high and rising need and cost of LTC, figuring out how to pay for it is critical. Care providers receive over 70 percent of their revenue from government sources, primarily Medicaid and Medicare. Medicaid pays for most long-term custodial care. Medicare pays for shorter-term sub-acute and rehabilitative care. Medicaid LTC reimbursement is notoriously meager, often less than the cost18 of providing the care.19 Medicaid funds 65.4 percent of nursing home patient days and contributes 49.6 percent of their revenue.20 Medicare reimbursement is more generous and helps to make up for losses from Medicaid, but Medicare faces serious solvency problems. Medicare has large and growing unfunded liabilities—$34.6 trillion as of October 2, 202221—and the Medicare Payment Advisory Commission (MedPAC) often recommends cutting reimbursement levels.22 23
The amount of LTC funded by private pay, including out-of-pocket expenditures and private health insurance, has declined steadily since Medicaid began paying for nursing home care in 1965. In 1970, patients privately paid 49.2 percent of nursing home costs, but today they contribute only 23.0 percent.24 Only 7.6 percent of nursing home revenues are from patients paying privately.25 Home care is similar. As of 2020 only 10.2 percent of home care costs were
paid out of pocket.26 The remainder came from public or private insurance.
Medicaid has a disproportionate impact on LTC. Although it paid only 42.1 percent of LTC dollars in 2020,27 Medicaid’s influence is much greater. The program covers 62 percent of all nursing home residents28 and 16.5 percent of assisted living residents,29 and it makes a rapidly growing contribution to home and community-based services (HCBS).30
How can Medicaid pay only two-fifths of LTC costs but cover three-fifths of the most expensive patients (i.e., those in nursing homes)? Three factors principally account for this incongruity:
- Costs are shifted from private patients. Medicaid provider reimbursements are roughly 70 percent of private-pay rates.31
- Medicaid LTC recipients are required to contribute most of their income to offset the program’s cost for their care.32 This can and occasionally does result in a Medicaid recipient’s income covering the entire cost of the care, leaving the nursing home in receipt of the low Medicaid rate even though Medicaid paid nothing.
- Medicare, which pays far more generously than Medicaid does for nursing home and home care,33 enables LTC providers to survive financially while most of their patients’ care is reimbursed at meager Medicaid rates.34
The impact of Medicaid LTC financing is substantially greater than the raw numbers suggest in ways almost never acknowledged in the literature. For example, most of the income Medicaid recipients contribute to offset Medicaid’s cost for their care comes from Social Security. Although Social Security is not usually considered a financing source for LTC, the fact is that it contributes very significantly, albeit indirectly as “spend-through.” Social Security spend-through refers to income most seniors collect in the form of Social Security benefits that they must contribute toward their cost of care when they receive LTC services paid for by Medicaid. There is very little in the literature about this source of LTC financing, although research from 20-30 years ago indicated it accounts for nearly half of reported out-of-pocket nursing home costs. Thus, Social Security spend-through amounts to nearly half of the $45.3 billion (23.0 percent) reported as “out-of-pocket” costs in 202035 as inferred based on Lazenby and Letsch (1989)36 and McCall (2001).37
This added dependency of LTC providers on Social Security and Medicare contributes to the fragility of the LTC financing system. If the Social Security and Medicare Part A trust funds expire as expected in 203538 and 2028,39 respectively, resulting in substantial cuts to those programs, LTC providers dependent upon those revenues will be in further financial peril.
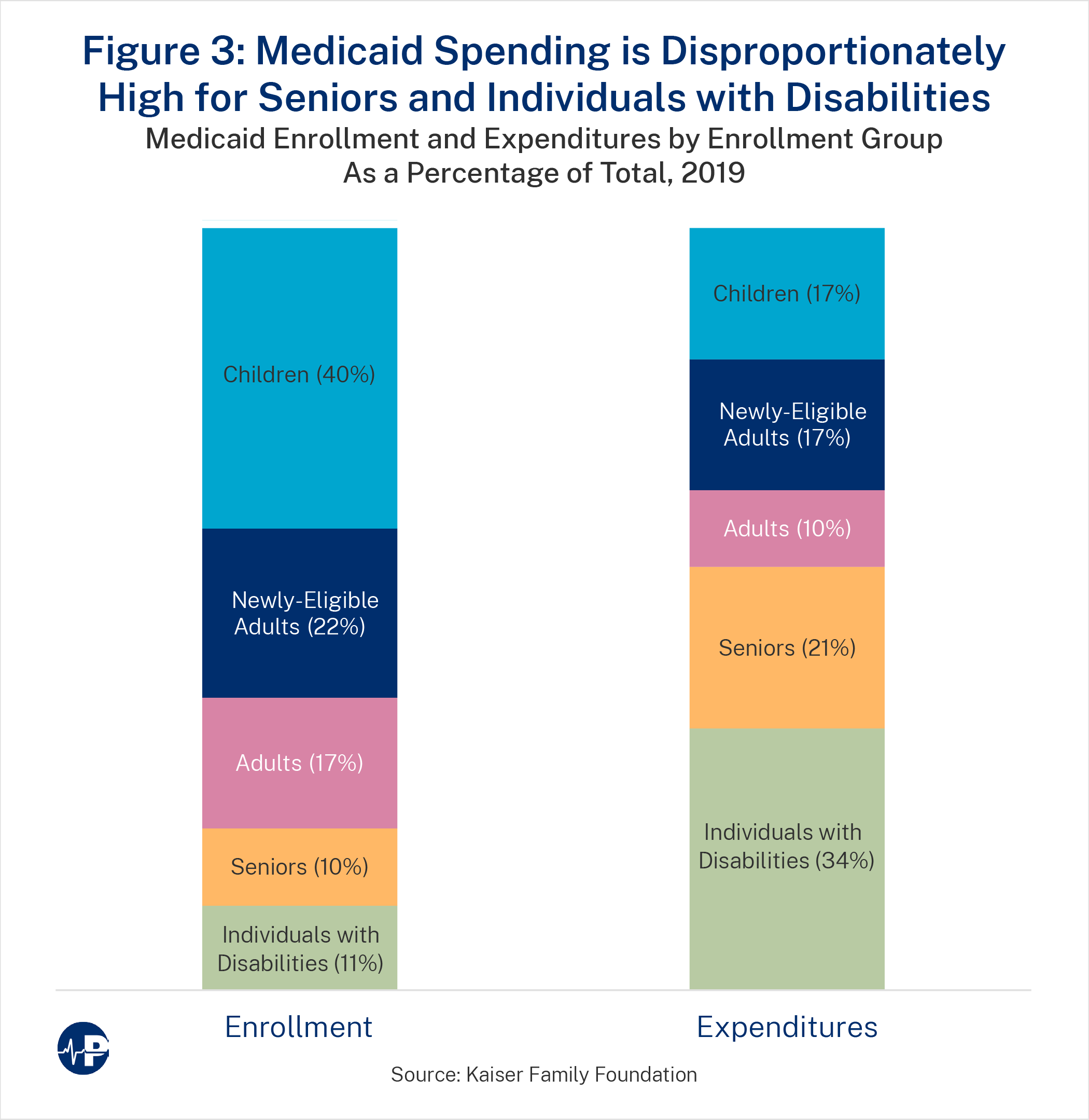
Likewise, LTC has a disproportionate impact on Medicaid. Despite a relatively small number of Medicaid enrollees using LTC services, the spending associated with these groups is outsized. As Figure 3 indicates, the aged and disabled who are most likely to use LTC were 21 percent of Medicaid enrollees40 but accounted for 55 percent of Medicaid expenditures in 2019.41 Furthermore, LTC users, who are 5.9 percent of enrollees, consumed 41.8 percent of total Medicaid benefit spending for both institutional and non-institutional LTC in 2013.42
The high cost of LTC, LTC providers’ heavy dependence on public financing at low Medicaid reimbursement rates, and LTC’s disappearing higher market-rate private revenue have serious consequences for care access and quality. People who need care often do not qualify immediately for the public programs that provide it. Yet they cannot afford to pay privately for care at market rates, at least not for very long. Underfunded nursing home and home health providers face labor shortages and wage pressures exacerbated by pandemic complications, including vaccine mandates and inflation. Direct caregivers are expected to do the hard work of attending patients for long hours at relatively low wages, so they are in short supply.43 44 Individuals, families, and friends fill the service gap by providing unpaid care. This often means foregone earnings, reduced leisure, and direct care expenses.
LTC History
The history of LTC involves a constant tension between public and private financing. Repeatedly, government interventions in the LTC financing system caused negative unintended consequences. In response, entrepreneurs attempted to ameliorate the problems but never solved them entirely.
For example, government involvement caused explosive costs and nursing home bias, impaired LTC financing, created caregiver shortages, hampered LTC access and quality, and obstructed promising private LTC insurance and home care services markets. In response, entrepreneurs developed more attractive alternatives such as assisted living and private-pay home care. But these alternatives struggled given the bias in policy toward nursing homes. Many wealthier consumers abandoned nursing homes for the alternative care settings even though they had to pay out of pocket. Most consumers remained in the dominant Medicaid-financed system. Because of competition with free or subsidized public LTC funding, private financing sources such as home equity conversion and private insurance were never able to take hold fully despite their obvious potential to mitigate the LTC funding shortfall.
Problem With the Current LTC System
Explosive Costs
Social services and benefit programs in the United States evolved gradually in the country’s first two centuries from a system based on British poor laws—“indoor relief” with many poor houses—toward a system based on cash relief payments.45 Cash payments from programs such as Old Age Assistance and Social Security gave people funds to spend on residential LTC, enabling the nursing home industry to grow rapidly.46 In 1960, the Medical Assistance for the Aged program made health care available to people 65 and older with low or moderate income and required state matching funds.47 The same Kerr-Mills statute radically changed eligibility for nursing home care by adding people who “were not sufficiently needy to qualify for cash assistance to cover their ordinary expenses, but who were unable to pay their medical expenses.”48
In 1965, the newly enacted Medicaid program dropped strict eligibility criteria, transfer-of-assets restrictions, and mandatory liens, which were commonplace in state programs previously.49 These changes expanded eligibility for government-financed LTC services. For its first 15 years, Medicaid explicitly permitted asset transfers for the purpose of qualifying for LTC benefits.50 Finally, Medicaid paid exclusively for nursing home care, incentivizing its use by covering “housing, food, housekeeping, and laundry services which were not covered for in-home services.”51
As a result of loose eligibility requirements and federal matching dollars for state spending, Medicaid LTC growth exploded,52 a bias toward nursing home services solidified,53 and private financing alternatives were crowded out.54 Policymakers have been trying to reverse the damage ever since by discouraging the program’s overuse through financial eligibility constraints and by diverting Medicaid financing toward HCBS.
Nursing Home Bias
Before the Great Society programs of the 1960s, small mom-and-pop facilities provided most formal LTC, and people generally paid out of pocket.55 Medicaid began funding nursing home care—including room, board, laundry, and custodial and medical care—shortly after its founding in 1965. To qualify, people could give away assets and income rarely mattered, because Medicaid was designed to help not only the poor but also the “medically needy,” meaning anyone with too little income to cover their LTC costs privately. Consumers responded predictably, taking advantage of the new subsidy. Why pay privately for LTC when the government provided generously? The nursing home business also responded, expanding and corporatizing rapidly.56 By paying exclusively for nursing home care, Medicaid created the institutional bias that has plagued LTC ever since.
Rebalancing to Home Care
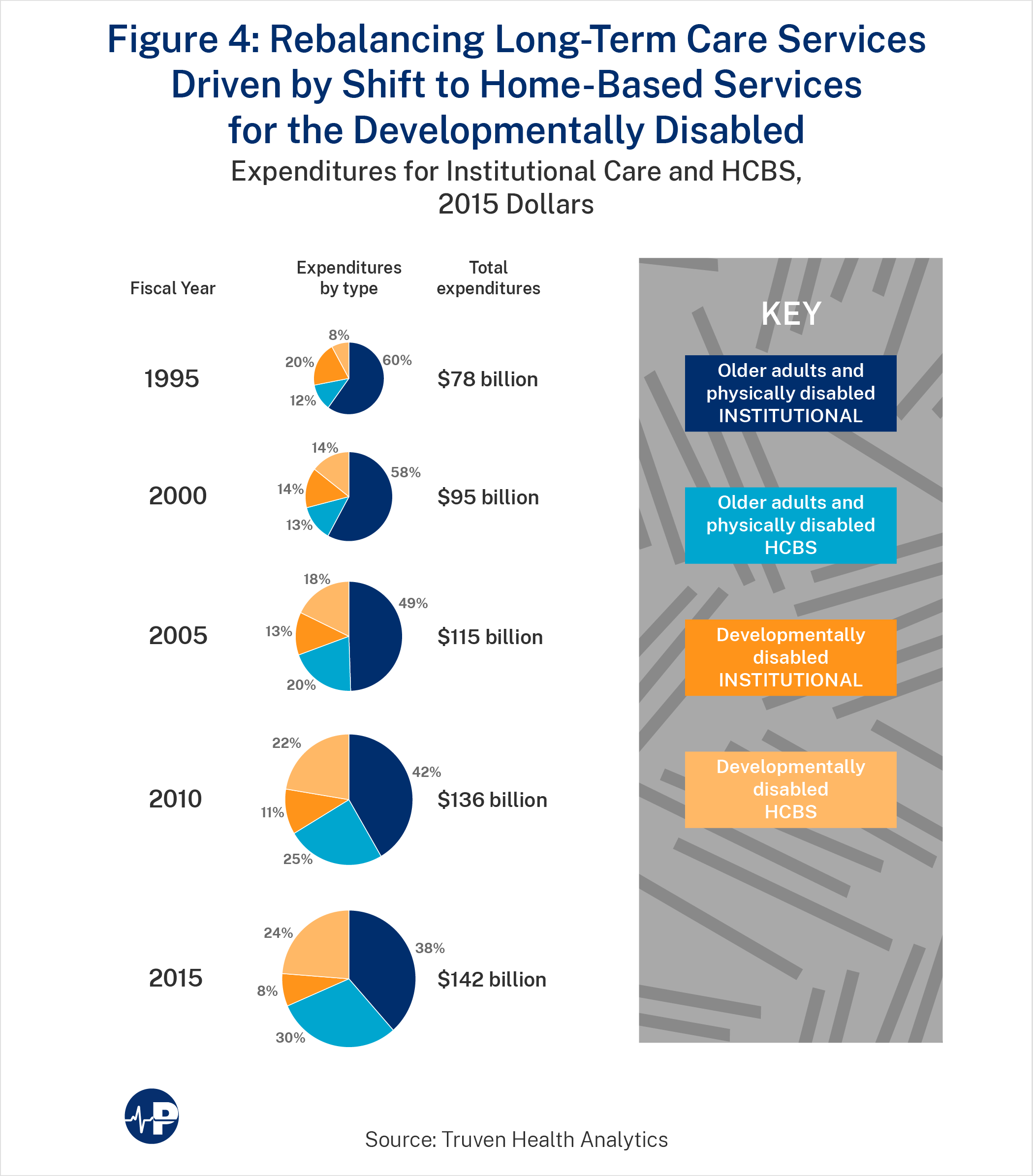
Analysts, advocates, and policymakers increasingly lamented Medicaid’s institutional bias. They attempted to move Medicaid financing away from nursing homes toward more HCBS. Since 1981, waivers have allowed states to circumvent Medicaid rules that require nursing home coverage but prevent home care options. All states have such waivers.57 A new initiative called “Money Follows the Person,” supported by several laws from 2005 through 2020, aimed to “increase the use of home and community-based services (HCBS) and reduce the use of institutionally-based services.”58 Over time, total Medicaid LTC spending has increased but has shifted proportionally from nursing homes to HCBS, as illustrated by Figure 4.
By 2016, 57 percent of overall spending was for HCBS, up from 18 percent in 1995.59
This shift to HCBS has favored the younger, developmentally disabled recipients over the elderly: 76 percent of Medicaid LTC spending for people with developmental disabilities was for HCBS, whereas only 44 percent of LTC spending for older people and younger persons with physical disabilities was for HCBS in FY2015.60 Mathematica found that the elderly’s share of HCBS spending for LTC slipped to 33.7 percent in FY2017 and 32.9 percent in FY2018, although several large states did not report data for those years, which probably reduced these amounts.61
Comparing 1995 with 2015 on Figure 4 reveals how much more the transition to HCBS has affected the developmentally disabled (from 20 percent institutional/8 percent HCBS in 1995 to 8 percent institutional/24 percent HCBS in 2015) compared to older adults (60 percent institutional/12 percent HCBS in 1995 to 38 percent institutional/30 percent HCBS in 2015).62
Due to a change of methodology in the latest report, this important distinction between Medicaid HCBS for the elderly versus younger, disabled recipients will no longer be tracked.63
Importantly, despite the shift from institutional services to HCBS, total public spending on LTC continues its substantial increase.
Thanks both to the popularity of HCBS and the government’s cost-neutrality requirement (i.e., waivered HCBS may not exceed what would have otherwise been spent on institutional services), access to Medicaid home care remains plagued by several problems, including:
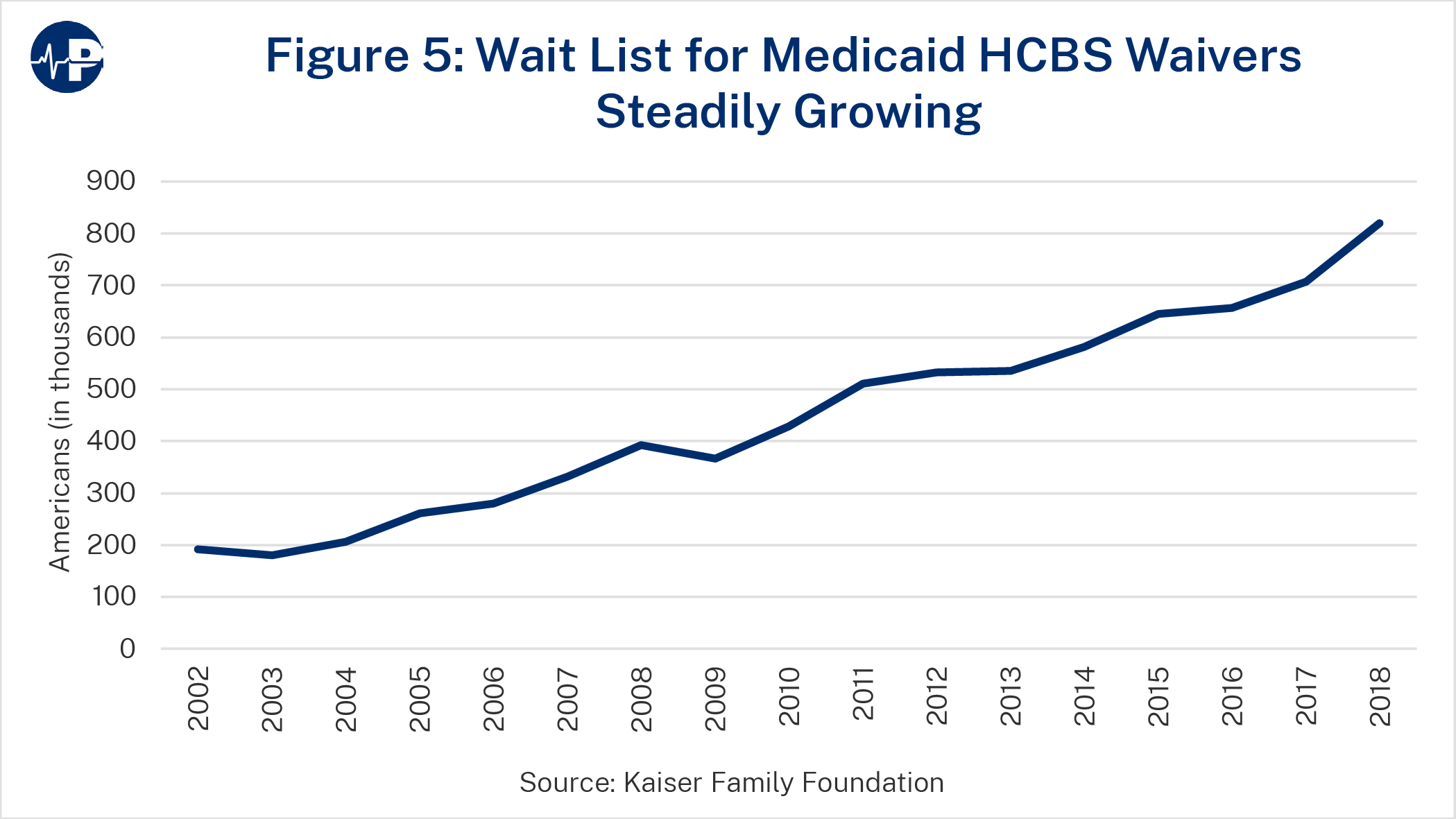
- long waiting lists, which totaled 665,000 people in 202064 (see Figure 565);
- low wages for workers;66
- worker shortages;67
- poor quality of care;68 and
- significant risk of waste, fraud, and abuse.69
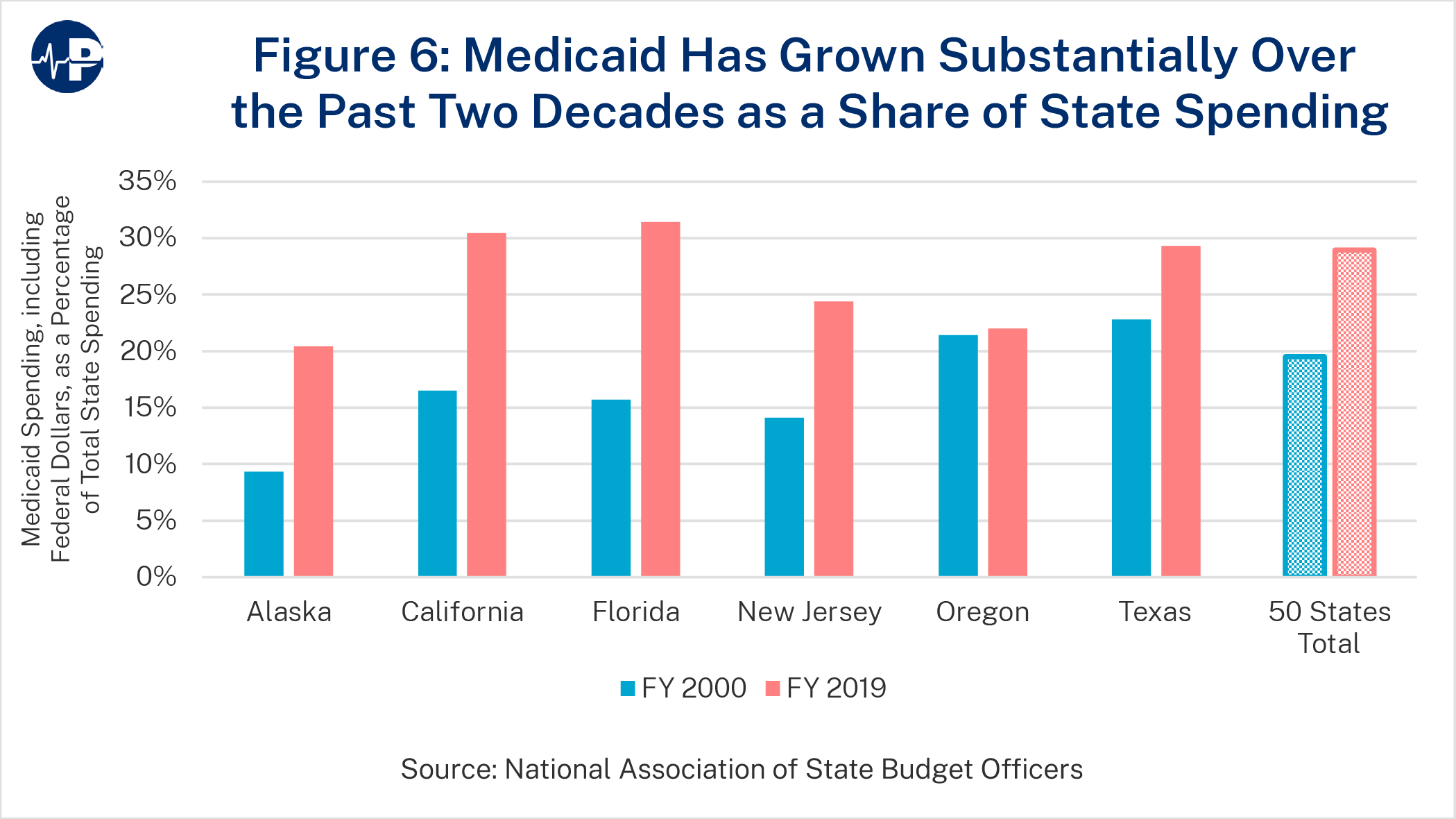
Despite long-standing claims that home care saves money compared to institutional care, this is not the case. Studies and practical experience showed that while home care was less expensive for some patients, it delayed but did not replace institutional care for many people.70 71 Consequently, despite a higher percentage of spending on home care, total Medicaid LTC expenditures for home care and nursing home care increase steadily year after year, as Figure 4 shows,72 further impinging on state and federal budgets, as Figure 6 shows. The bottom line is that what has happened is not so much rebalancing from nursing home care to HCBS as rapid expansion of HCBS while nursing home expenditures remained relatively flat during FY2012-FY2015.73 So transitioning from nursing home care to HCBS has not proved to be the panacea it was long hoped and expected to be for reducing Medicaid budgetary pressure.
Inadequate LTC Financing
Rapidly increasing Medicaid LTC expenditures, especially in the early years, motivated government to contain them in various ways. Figuring “they can’t charge us for a bed that doesn’t exist,” certificate of need (CON) laws were passed that restricted the construction of new nursing homes and effectively capped the number of nursing home beds in many states.74 The nursing home lobby did not object. CON laws created an artificial barrier to market entry, thus securing a government-enforced monopoly for nursing homes already in place.75
But with their market expansion restricted, nursing homes sought to grow their profits by raising the rates they charged state Medicaid programs. The federal government and states responded by capping Medicaid rates. These capped rates created the large differential between market-based private-pay nursing home payments (national average: $297 private room; $260 shared room) and Medicaid rates ($208; $182, respectively), which are often less than the cost to provide the care and average about 70 percent of private rates today.76
These higher private pay rates created an additional incentive for people to find ways to qualify for Medicaid. Magazine articles, popular books, and formal legal literature proliferated explaining how families can organize their income and assets to qualify for Medicaid LTC benefits without impoverishment. Nursing homes became increasingly dependent on Medicaid, lost most of their higher private payers, and relied more and more on Medicare’s higher reimbursements for shorter-term sub-acute and rehabilitative care.
Poor Access and Quality
Demand for Medicaid nursing home care grew rapidly. By the early 1980s, nursing homes were 95 percent occupied77 at a time when hospitals were only 78 percent full.78 If a nursing home was willing to accept Medicaid’s low reimbursement rates, it could fill all its beds, almost regardless of the quality of care it offered. Consequently, care quality collapsed in principally Medicaid-financed nursing homes.79 Surveys showed and continue to show80 that many people would rather die than reside in a Medicaid nursing home. Congress responded in the Omnibus Budget Reconciliation Act of 1987 (OBRA ’87), also known as the Nursing Home Reform Act, by mandating more caregiving staff, better training, and higher pay. But OBRA ’87 provided no extra funds to support these new requirements, and quality remained dubious decades later.81 In 2017, on the 30th anniversary of OBRA ’87, the Kaiser Family Foundation published a review of HCBS and nursing home quality highlighting ongoing deficiencies and inadequate tracking.82
Caught between inadequate reimbursement and quality mandates, nursing homes and their trade associations began suing for higher Medicaid reimbursement.83 They won most of those lawsuits by appealing for relief under the Boren Amendment of 1980, which ensured “reasonable and adequate” Medicaid reimbursement rates to provide care “in conformity with applicable state and federal laws, regulations, and quality and safety standards.”84 In the end, Congress repealed that part of the Boren Amendment, leaving no floor under Medicaid nursing home reimbursement rates. Thus, the quality problems and resulting caregiver shortages have persisted to the present.85 The Biden administration appears to be making the same mistake now by demanding minimum staffing requirements, stronger regulatory oversight, and better public information about nursing home quality86 without providing sufficient additional funding to support the new requirements.87
Today, in the ongoing COVID disruption, access to and quality of Medicaid LTC are increasingly problematic. Besides long wait lists for home care, Medicaid nursing home beds are scarce due to staff shortages, causing facilities to limit admissions.88 Discrimination against patients who rely on Medicaid payments is also a serious and growing problem.89
Disappearing Private Revenue
Private-pay rates are often one and a half times as much as what Medicaid pays. Given the ease with which people could qualify for Medicaid—especially in the early years—fewer and fewer patients and their families were willing to pay out of pocket for services they could get from Medicaid for free or with a large subsidy. Out-of-pocket expenditures for nursing home care plummeted from 49.2 percent in 1970 to 23.0 percent in 2020.90 Notably, about half of those out-of-pocket costs for nursing home care come from Social Security and other income that Medicaid recipients are required to contribute toward their cost of care—that is, not from spend down of personal savings.91 In 2011, CMS changed the National Health Expenditure Account categories to add Continuing Care Retirement Communities (CCRCs) to Nursing Care Facilities. This change had the effect of reducing Medicaid’s reported contribution to the cost of nursing home care from over 40 percent in 2008 to under one-third (32.8 percent) in 2009. Because CCRCs are almost entirely private pay and they cover independent and assisted living as well as nursing home care, this definitional change made Medicaid’s contribution smaller for this category and out-of-pocket expenditures greater. Thus, for nursing homes only, excluding CCRCs, Medicaid is a bigger contributor and out-of-pocket spending a smaller contributor than the data for the combined category suggest.
Out-of-pocket expenditures for home-based LTC services are also low: about 10 percent of total spending in 1970 and today.92 Even less are out-of-pocket expenditures for HCBS, residential, and personal care at only 3.2 percent.93
In all three categories, Medicaid and Medicare expenditures increased significantly from 1970 to 2020: from 26.8 percent to 47.1 percent for nursing homes and CCRCs; from 33.4 percent to 66.1 percent for home health care services; and from 11.8 percent to 60.5 percent for other health, residential, and personal care services.
Clearly, the increasing availability of Medicaid and Medicare to fund LTC and related health care expenses created a strong disincentive for consumers to plan for the risk and cost of someday needing extended care.
Paid Caregiver Shortages and Overwhelmed Family Caregivers
Both nursing home and home care workers generally receive lower wages than do their peers with similar credentials.94 An LTC system dominated by public financing at less than the cost of providing the care simply cannot attract enough caregivers.95 By paying LTC providers so poorly, Medicaid created the caregiver shortages and quality deficiencies that have characterized America’s LTC system ever since. Long-term caregiving—which involves monitoring, turning, lifting, transferring, and bathing often helpless patients—is challenging and often dangerous work.96 Finding people to do that work for low wages proved daunting. In the throes of the COVID pandemic, employing and retaining enough paid caregivers became almost impossible.
Too Many Dual Eligibles
Easy access to Medicaid nursing home care once care is needed reduces the necessity to plan ahead to pay privately if the need arises and causes several other distortions in the LTC market. The dual eligible population—people eligible for Medicare and Medicaid simultaneously—grew to alarming levels. Dual eligibles are the most expensive beneficiaries of both programs. Twenty percent of Medicare beneficiaries and 15 percent of Medicaid recipients are duals, but they consume 34 percent of Medicare and 33 percent of Medicaid expenditures, respectively.97 Nevertheless, their care outcomes are poorer.98
Duals are 5.0 times more likely to have a disability and 2.6 times more likely to be of minority race or ethnicity than their non-dual counterparts. They have markedly worse health outcomes, being two times more likely to be hospitalized or die after adjusting for comorbidities, than nondual beneficiaries.99
People age into Medicare at 65, but they often become dual eligibles because Medicaid is relatively easy to qualify for financially when care is needed many years later. Diverting people earlier in their lives from later dependency on Medicaid could substantially reduce the number and cost of dual eligibles in later years. Such diversion would require getting consumers concerned and acting about LTC risk and cost much earlier in their lives. Part 2 of this series will propose a plan to achieve that objective.
The next paper (Long-Term Care: The Solution) will explain the necessary steps to end the government’s distortions of the LTC market and to incentivize people to prepare financially for the future.
Many Problems Driven by Medicaid’s Financial Structure
Medicaid’s financing system, in which the federal government matches state expenditures at a minimum of 50 percent, creates an incentive for states to maximize Medicaid without being cost conscious. States with lower per capita income receive a more generous federal match. For every dollar states spend on Medicaid, they draw at least one additional dollar from the federal government, and on average states draw two federal dollars for each dollar of state spending with state resources.100
To generate extra federal contributions, states often charge their LTC providers special taxes, spend that money through Medicaid, obtain matching funds from the federal government for that expenditure, and often reimburse the providers in whole or in part for the tax. This “provider tax” system has the effect of increasing the cost of Medicaid to federal taxpayers and generating a windfall of extra federal revenue for states.101 Famously, the state of New York turned Medicaid into a verb by “Medicaiding” all sorts of state activities to pull in extra federal funds.102
HOW THE PRIVATE SECTOR AMELIORATES PROBLEMS THE GOVERNMENT CAUSES
Private consumers and companies responded creatively to the nursing home bias, exploding costs, poor quality, caregiver shortages, and excessive strain on family caregivers that Medicaid created. They partially repaired the damage from government policies and regulations that created the problems.
Assisted Living
In the 1980s, a new venue of care evolved called assisted living.103 Characterized by attractive facilities offering private rooms and lighter, non-medical, custodial caregiving, the assisted living model quickly gained popularity. While assisted living gave consumers a choice, its growth was hamstrung by the availability of free or highly subsidized nursing home care provided by Medicaid. Over time, struggling to fill the industry’s rapidly increasing capacity, assisted living providers began accepting residents whose bills were paid by Medicaid. They reckoned that it was better to accept Medicaid’s impecunious payment rates than to have an empty unit. Today, 16.5 percent of assisted living residents rely on Medicaid.104 The assisted living business is gradually following nursing homes down a primrose path of dependency on public assistance.
Private Home Care
Another way consumers and entrepreneurs have responded to ease LTC problems caused by Medicaid is through the creation of a market for privately financed home care. As an example, Amada Senior Care, recognizing that their service, however critical, is also hard for families to afford, pursues creative ways to help people find the funds to pay their fees. The company seeks potential customers who already own private LTC insurance that covers home care, as most such policies do. Amada works closely with LTC insurance carriers and distributors to ensure that its insured customers receive all the benefits they are entitled to under their policies. As many older people are house rich but cash poor, Amada helps prospects and customers who own homes utilize reverse mortgages to generate the cash flow to cover their home care costs. Likewise, older people often own life insurance policies with considerable cash value. Amada assists them to find life settlement opportunities, freeing up funds to pay for its home care services. In a free market, companies have strong incentives to help their customers afford their products and services. In markets dominated by public financing, all financial incentives lean toward adapting to rules and regulations imposed by the controlling government agency whether they redound to consumers’ benefit or not.105
Other Market-Based Approaches
The private sector is developing other ways to ameliorate the damage Medicaid has done. For example, many businesses are trying to improve HCBS:
Walmart is among a growing legion of retailers including Amazon, CVS, Walgreens and Dollar General that are moving aggressively into healthcare, with most offering services aimed directly at the home. Walmart’s online Wellness Hub sells products and services, including diagnostic testing.106
Villages are “membership organizations created by and for older adults whose purpose is to help people live independently while staying in their own homes. Typically, villages help arrange services for members: a handyman to fix a broken faucet, a drive to and from a doctor’s appointment, someone to clean up the yard or shovel the snow. Volunteers do most of the work.”107
Imagine the possibilities that entrepreneurs and investors could create to provide the kinds of LTC products and services consumers prefer if public policy did not channel them into providing only those products and services for which government pays.
Private Insurance Stifled by Medicaid
LTC insurance carriers, distributors, and producers struggled to market the product despite obstacles put in their way by crippling public policies. Medicaid gave away the LTC protection that the industry was trying to sell. Medicaid benefits became available long after the insurable event occurred, thus desensitizing future potential buyers of the product about the risk. Brown and Finkelstein “estimate that Medicaid could explain the lack of private long-term care insurance for about two-thirds of the wealth distribution, even if no other factors limited the market’s size.”108 The Federal Reserve has forced interest rates down since the 1980s and to near zero in the past decade,109 making it impossible for insurers to receive the returns on their reserves that they would need to pay benefits when they come due. With very little long-term morbidity experience to base premiums on, carriers underpriced early products, which were nevertheless still crowded out by the available public financing from Medicaid.
The insurance industry adapted creatively, designing new kinds of LTC coverage that would pay whether the insured incurred an LTC cost or not, such as hybrid policies combining annuities or life insurance with LTC protection. The federal government has made half-hearted efforts to encourage private LTC insurance—such as tax deductibility of premiums that proved unavailable to most seniors and the unsuccessful “LTC Partnership” program to forgive Medicaid estate recoveries, which were easily avoided and only sporadically enforced anyway. Despite those efforts, easy access to Medicaid ruined the possibility that private insurance could play a major role in funding LTC. The number of carriers offering the product plummeted from over 100 to under a dozen.
Confronted with too few reserves to meet contractual obligations to beneficiaries, private LTC insurers raised their premiums to make up the difference. That cost them the good will of prospects and the enmity of insureds who endured substantial premium increases. But unlike the government programs that pile up debt with politicians seeming incapable of shoring up their reserves, private insurers did the right thing. Importantly, private insurance will pay when claims occur. The ability of Medicare and Social Security to pay full benefits in the future is dubious.
Because of the problems Medicaid created in LTC, being able to pay privately in order to access quality care in the most appropriate venue has become critically important. Nursing homes eagerly welcome patients who can pay privately because they pay higher rates than Medicaid recipients do. Assisted living remains mostly private pay. To get into the nicest skilled nursing and assisted living facilities, people must be able to pay privately, at least temporarily. To avoid the kind of small congregate home care settings of dubious quality or low-quality nursing homes for which Medicaid primarily pays, consumers need to be able to pay privately for a topline home care provider.
The latest Genworth Cost of Care Survey shows substantial increases in the cost of all three levels of care.110 Nursing home care is $94,900 annually for a semi-private room; assisted living is $54,000 per year; homemaker and home health care services are $26 per hour and $27 per hour, respectively.111 Between wage pressures to attract scarce caregivers and economy-wide inflation, these costs will likely increase significantly. The 5 percent cost-of-living increases built into many early LTC insurance policies, which seemed excessive during recent low inflation, may prove inadequate going forward due to rapidly increasing inflation.
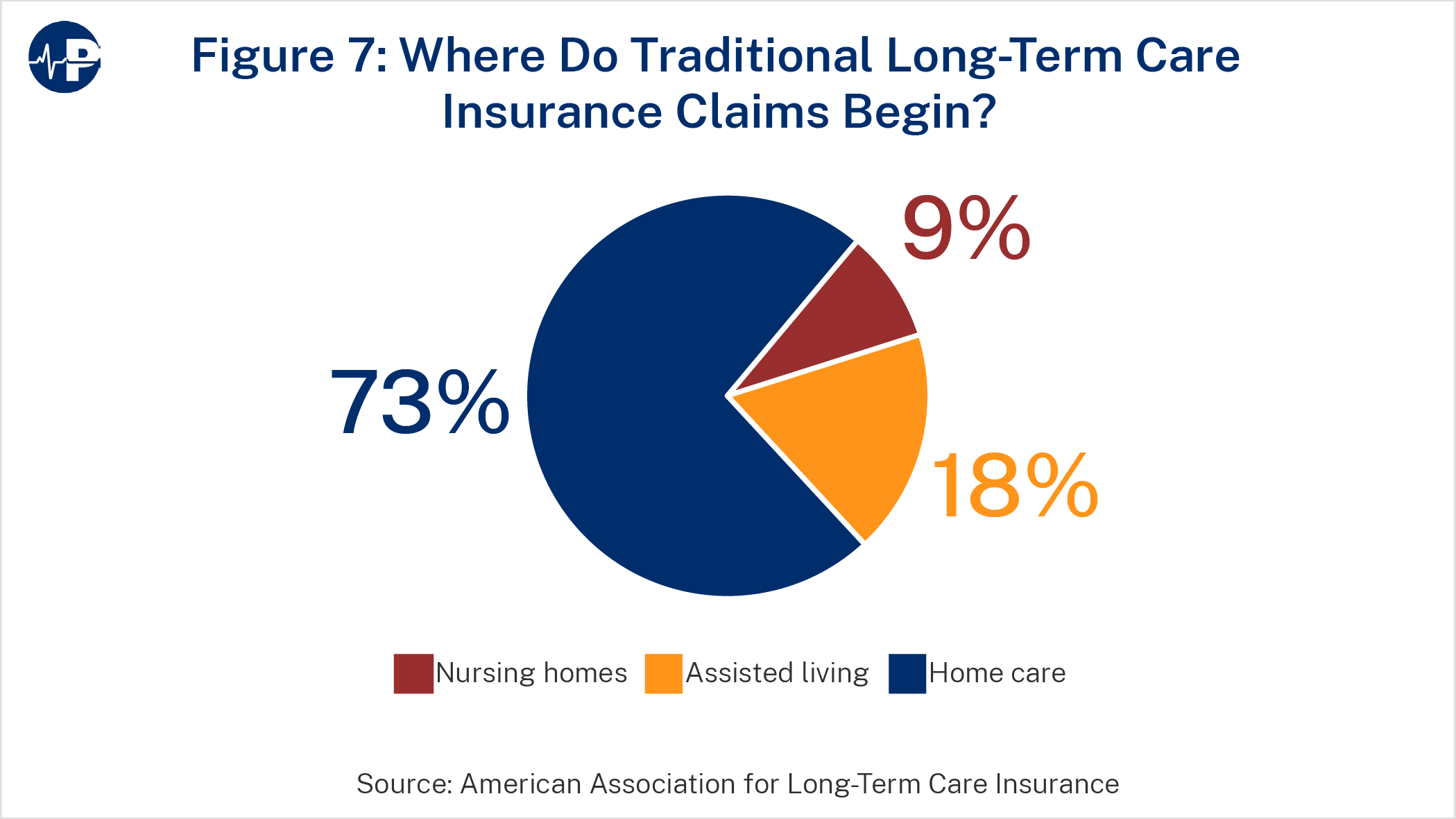
Increased use of private LTC insurance could have prevented much of the damage Medicaid caused, freeing millions of Americans to choose the care venues they prefer. Data indicate that the vast majority (73 percent) of new LTC private insurance claims occur while the patient is still at home. Medicaid, on the other hand, mostly pays for claims occurring in nursing homes and usually pays for home care only after the recipient has waited for a long time.
Growth of Managed Long-Term Services and Supports
Another aspect of Medicaid LTC that the private sector has impacted, though with only questionable benefit, is the burgeoning expansion of Managed Medicaid LTSS, or MLTSS.112 MLTSS refers to the delivery of LTC through capitated Medicaid managed care programs.113 It is based on the idea that private companies can provide better care for less cost by receiving a per-person rate across a coverage group. As of 2021, 24 states operated such programs, compared to eight in 2004.114 The hope is that managed LTC can promote wellness and save money by reducing institutionalization through increased home- and community-based care. The model is not yet proven. MLTSS places an extra level of administration and compensation between LTC patients and providers, often reducing providers’ reimbursement.115 The Government Accountability Office found “significant problems with the quality of care provided through these contracts” in the six states it reviewed.116
The Fallacy of Impoverishment
The biggest public misperception, shared by average citizens as well as many experts, is that Medicaid LTC eligibility requires impoverishment. It does not. There is no evidence that it does. Researchers—who routinely claim that wide swaths of the American public spend down catastrophically for LTC before becoming Medicaid eligible—never cite empirical evidence. If Medicaid eligibility did require impoverishment, the public would seek to avoid catastrophic LTC spend down by saving or insuring against the risk. But because it does not, most people ignore LTC risk until they need expensive care. At that point, the only way to avoid paying for care privately is to qualify for Medicaid. Both patients and their adult child heirs have a strong incentive to follow this path and frequently do.
Why does the myth that Medicaid requires impoverishment persist despite the lack of evidence for it? Medicaid law and regulations appear to require financial destitution in order to qualify. The law limits income to $841 per month—the Supplemental Security Income (SSI) monthly payment for a single person—and caps assets at $2,000. Only the truly poor could qualify if these were really the rules that applied.
But the practical reality is very different.117 Most states allow Medicaid applicants to deduct their health and LTC expenses from their income before applying the income eligibility criterion. As most older people in need of LTC have very high health and LTC expenses, this policy allows people with incomes well above the median to qualify. Other “income cap” states apply an income limit of 300 percent of the SSI monthly payment, or $2,523 per month. Income above that amount may be diverted into a Miller income diversion trust, which then pays the Medicaid provider’s fee with any excess devolving from the trust at death to the state.118 A common rule of thumb is that anyone with income below the cost of a nursing home is eligible based on income. With nursing home fees averaging nearly $8,000 per month—nearly quadruple the median income of an elderly person ($2,283 per month119)—almost all older Americans are eligible for Medicaid based on the income rules.120
The situation with asset eligibility is similar. Analysts often ignore or discount the difference between “countable assets,” which are limited to $2,000, and exempt assets, which have no set limit. The reason most elderly Americans qualify for Medicaid LTC without having to spend down their wealth, despite the common assumption that they do and must, is that the vast majority of that wealth is held in assets that are exempt from the Medicaid asset test. Exempt resources include home equity—up to $636,000 in most states and $955,000 in the rest except California, which applies no limit at all in open defiance of federal law.121 Many other assets are exempt122 without any dollar limit, including one vehicle, home furnishings and personal belongings (including family “heirlooms,” regardless of when they were purchased), prepaid burial plans, term life insurance, one business (including the capital and cash flow), and individual retirement accounts if they are in payout status (all accounts are in payout status for people 72 years and older due to the required minimum distribution rules).123 It is very easy—and universally recommended by books and legal experts—to convert countable assets into exempt assets. In fact, state Medicaid eligibility workers routinely advise applicants to reduce their countable resources by purchasing exempt assets, especially prepaid burial plans for the applicant and immediate family members, and other items such as televisions or furnishings for their new Medicaid-financed assisted living or nursing home rooms.
Why People with Sizeable Estates End Up on Medicaid
Medicaid is a welfare program, meaning that it is means-tested public assistance.124 How do people who possess substantial incomes and assets qualify? Consider a hypothetical example of an elderly couple with median income and assets.
John and Mary Smith were born in 1937, when life expectancy was 58 years for men and 62 years for women.125 They married in 1959, started a family, and began payments on a home. Theirs was the American dream—happiness and prosperity—until the 2010s. At age 80, with a life expectancy of an additional eight years,126 John was stricken by Alzheimer’s Disease.127 After a gradual onset, he began to require almost full-time care. Even with daily help from a home health aide ($27/hour)128 and the couple’s adult children—in their late 50s themselves—the responsibility finally overwhelmed Mary. By 2020, the family concluded that institutional care could no longer be postponed.129
Bob, the couple’s first child and a successful businessman, did some research. He located several excellent LTC facilities but was alarmed to learn that nursing homes charge over $100,000 per year for a private room.130 Even the more attractive assisted living facilities offering less skilled care would cost half that or more. Bob knew his father could easily live several more years.131 With his mother getting frailer every day, their combined care costs would consume his parents’ annual income of $34,925132 (mostly Social Security and an annuity) and in time their entire financial assets. Their main assets totaled $235,000, which included a home with no mortgage worth $148,000133 and roughly $87,000134 in retirement savings—comprised of $25,000 in stocks, bonds, and certificates of deposit, plus their individual retirement accounts (IRAs)—totaling $62,000.135
Bob thought that Medicare, which his father had already had for 15 years, would cover these expenses and ease the burden. When Bob visited the local Social Security office, however, he learned that Medicare does not cover custodial LTC.136 He checked his parents’ Medicare supplemental insurance policies and found that they were no help either.137 Furthermore, the couple had not purchased a private insurance policy that would have covered custodial LTC. They did not know they were unprotected,138 and no one ever tried to market such a policy to them.139
As his worry increased, Bob got some advice from a colleague who had been through the same wringer. “Talk to the people at the Department of Public Assistance about Medicaid,” she said. She explained that Medicaid has its shortcomings but might be a big help. Somewhat abashed, Bob arranged an appointment with a Medicaid eligibility worker. He received some good news and some better news. First, income would be no problem. Medicaid doesn’t count Mary’s annual $5,000 Social Security income because she receives it in her sole name, and John’s remaining income of $29,925 (or $2,500 per month) would not disqualify him because his private health and LTC costs would be deducted before comparing the remainder ($0) to the state’s $841 monthly income standard. He’d also be allowed to keep a $30 per month personal needs allowance while in the nursing home. Bemused, Bob realized that if his father’s income had been much higher—say, $8,000 per month—he still would have been eligible for Medicaid after the state deducted his monthly out-of-pocket nursing home bill of $8,500.
The better news Bob received was that his father would immediately pass the asset test for Medicaid eligibility. None of his resources was disqualifying. The eligibility worker explained that the couple’s home was exempt. In fact, John and Mary could have had over four times their actual home equity, up to $636,000, and John would still have qualified. On top of that, Mary’s IRA funds held in her own name and John’s IRA funds—currently in “payout status” because of his required minimum distribution—were exempt.140
To prevent “spousal impoverishment,” Medicaid allows the community spouse (Mary) to keep half the couple’s joint assets but at least $27,480.141 So their combined assets of $25,000 would all go to Mary, leaving John nothing and therefore eligible for benefits. The eligibility worker did explain that any resources left over after John’s passing would be vulnerable to recovery from his estate to cover the cost of his care. But that would happen only if Mary predeceased him. Otherwise, her own estate could be liable later, but few states pursue “spousal recovery,” so they and their heirs would likely never be affected by Medicaid estate recovery.
Relieved, but with his interest piqued, Bob did some more research. What he found surprised him. His parents possessed almost exactly the median wealth of people their age. But if they had much greater net worth of $790,000,142 they could still have qualified for Medicaid LTC benefits almost as easily. Deducting home equity of up to $636,000 leaves $154,000. Assuming none of that remainder is held in exempt IRAs or other noncountable resources,143 it is all countable. Mary’s Community Spouse Resource Allowance144—the amount of their combined assets she can keep—is one-half of $154,000 or $77,000, which leaves John the same amount, $77,000. That is $75,000 over Medicaid’s $2,000 countable asset limit. The eligibility worker would set up a “spend down” plan for John based on the average cost of a nursing home in the state. If that cost were $7,700 per month, John would become eligible for Medicaid in 10 months ($77,000/$7,700). Not bad, but this is where Bob discovered that there are many legal methods to avoid Medicaid asset spend down altogether.
On a tip from a colleague, he did an internet search for “Medicaid planning” and discovered dozens of law firms that specialize in helping affluent clients self-impoverish artificially. He also found a vast formal legal literature as well as numerous popular books and articles on the topic. It turned out that using that last $77,000 in the example without having to spend it on LTC as intended by the state and federal Medicaid program was very easy. The couple could buy a new car, since one car is exempt regardless of value. If they had a mortgage and their home equity was below the $636,000 limit, they could pay it down. They could buy unlimited personal belongings or home furnishings, all of which are exempt in unlimited amounts. The most common way to reduce countable assets, a method even recommended routinely by Medicaid eligibility workers themselves, is to prepay burial expenses. Medicaid planning attorneys give their clients long checklists of exempt assets and encourage them to use as much of their countable assets as possible to purchase things that will not interfere with their eligibility.
The one fly in the ointment Bob found was that Medicaid has a bad reputation for providing poor quality care. “Who would want to go to a welfare-financed nursing home or wait in a long line145 for rare Medicaid home care slots?” he thought. Then Bob spoke with an elder law attorney who has specialized expertise on this subject. He said, “We advise all our clients to hold back enough cash to pay privately for a few months. We call it key money. The best facilities roll out the red carpet for private payers, because they can charge them half as much as Medicaid pays. When we flip the switch and start Medicaid, there is nothing the providers can do. State and federal laws prohibit expelling residents because their source of payment changes.”
“Heck of a way to run a railroad,” Bob thought. “It’s welfare for the well-to-do, and it’s set up so only they get the best care, and the poor, who lack ‘key money,’ are shunted into the welfare homes.”
Beyond these already generous financial eligibility limits, the Medicaid law and regulations contain many “loopholes” that allow even very affluent people to qualify for the program while preserving all or most of their wealth. Special legal experts known as elder law attorneys or Medicaid planners employ “Medicaid friendly” annuities, Medicaid asset protection trusts, modern and reverse half-a-loaf strategies,146 and other sophisticated techniques to pry open restrictions intended to target Medicaid to the needy so that their well-to-do clients can qualify. Medicaid planners also counsel clients on how to avoid Medicaid’s estate recovery mandate, which is relatively easy to do and facilitated by the requirement’s generally weak enforcement by state Medicaid programs. Prosperous people who work routinely with financial planners, accountants, and lawyers on their estate planning learn about the importance of LTC early enough to transfer their assets to the next generation five years before requiring LTC. Assets transferred outside that five-year window, no matter how large, are not counted for purposes of determining Medicaid eligibility.
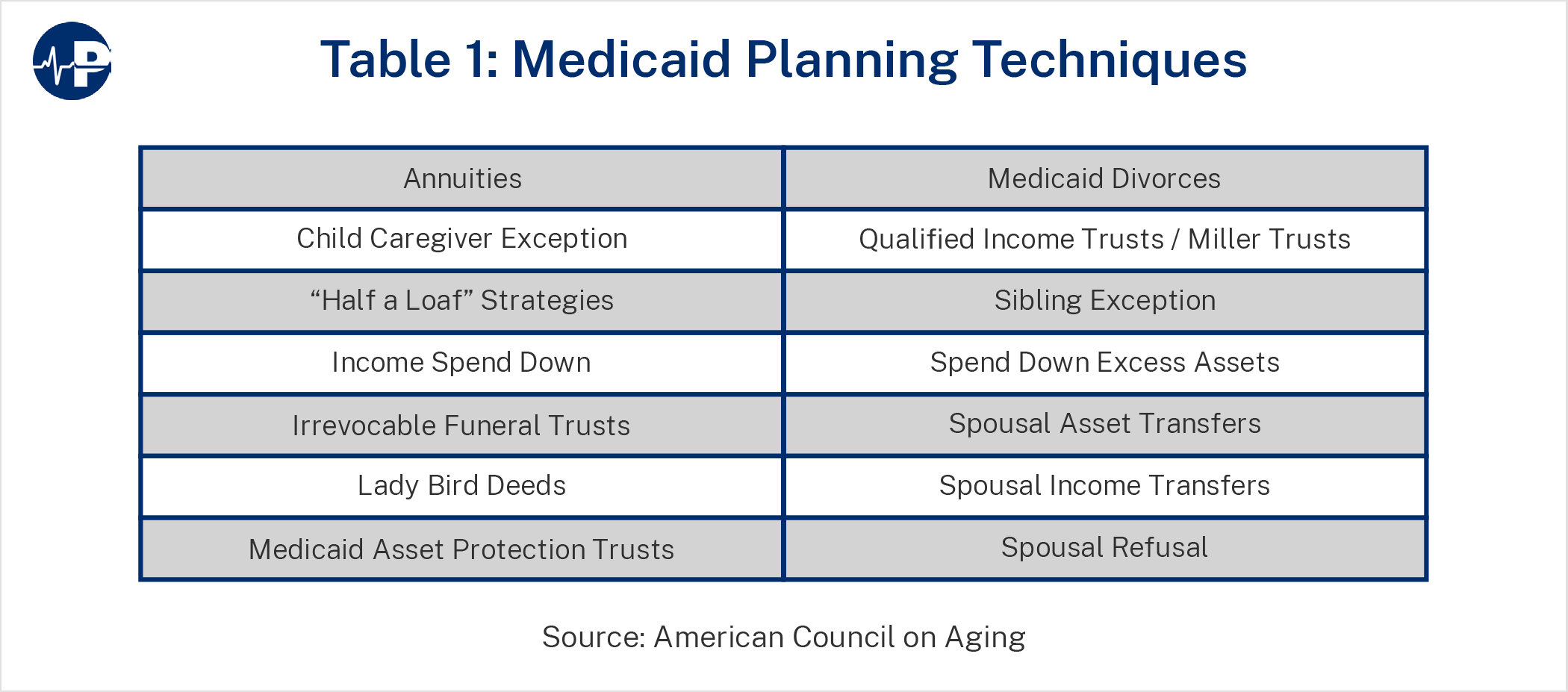
Some of the strategies used to qualify people for Medicaid LTC benefits without their having to spend down resources for care are listed in Table 1.147
Medicaid LTC eligibility workers and supervisors often complain that the income and asset restrictions they are required to enforce treat truly needy people more harshly than they do other more prosperous applicants. For example, a New York Medicaid assistant administrator from Long Island testified before Congress in 2011 that about 60 percent of applicants do some form of Medicaid planning:
It is not at all unusual to encounter individuals and couples with resources exceeding a half million dollars, some with over one million. There is no attempt to hide that this money exists; there is no need. There are various legal means to prevent those funds from being used to pay for the applicant’s nursing home care. Wealthy applicants for Medicaid’s nursing home coverage consider that benefit to be their right, regardless of their ability to pay themselves.148
Analysts who downplay the role of Medicaid planning in expanding eligibility and costs rarely acknowledge the vast formal legal literature describing and advocating methods to artificially impoverish clients to qualify them for assistance. They dismiss Medicaid planning as something the affluent would not do because of the program’s poor reputation,149 but they ignore the ways Medicaid planners get special treatment for their clients by withholding “key money” to buy their way into the best LTC facilities. Medicaid planning clients crowd out the poor from the best facilities because they can afford to pay privately at market rates for a time, making them prime candidates for admission at revenue-starved nursing homes and assisted living facilities. After a short period as private payers, the advisers convert their clients to Medicaid. The public is aware of the key money trick, as several answers to an “AgingCare GoFundMe” query indicate.150
Easy access to Medicaid LTC benefits once care is needed has had the effect of desensitizing the public to LTC risk and cost. Most people ignore LTC until they need it. At that point, Medicaid’s many deficiencies seem less onerous than the prospect of paying catastrophic LTC costs out of pocket. Unfortunately, the way the system works is that people with little wealth, low incomes, and scant exposure to legal and financial advice are quickly wiped out by Medicaid’s austere financial eligibility rules. But those with more wealth and higher incomes who are accustomed to working with legal and financial professionals learn how to preserve their wealth, qualify for Medicaid, and use key money to access the best services and facilities. Medicaid’s more favorable treatment of affluent people in terms of eligibility and access has led recently to charges of structural racism.
Structural racism in coverage and financing has created a two-tier system of racially segregated care in which minority people receive poorer-quality care.… Inequities in nursing home care provide a particularly vivid example.… Stark racial segregation in nursing homes persists today.151
Because of the fallacy of impoverishment’s predominance among scholars—and the convenience of using it to condemn the current system while promoting a new universal compulsory LTC program—we have little hard evidence about Medicaid LTC overuse. Studies that could produce the evidence are rare. In 2012, however, four members of Congress queried all state governors about Medicaid planning. Here are some examples of the replies they received:
- North Dakota: A couple with $700,000 in liquid assets qualified for Medicaid LTC benefits by purchasing a more expensive house, a car, and an additional annuity while receiving $8,000 per month from pensions, Social Security, annuity payments, and oil lease money. Another couple had more than $528,000 in assets but qualified when the community spouse bought a new home, a new car, and two annuities worth $240,000 and then applied for Medicaid to pay the institutionalized spouse’s nursing home costs.
- Wisconsin: An ill spouse transferred $600,000 to the community spouse, who refused to sign the Medicaid application, making the ill spouse eligible for Medicaid because “interspousal transfers are not considered divestment.”
- New York: Using promissory notes, immediate annuities, and spousal refusal, affluent LTC Medicaid applicants qualify while retaining unlimited assets. This occurs even when the state has legal recourse, because “Medicaid does not have sufficient resources to pursue all these cases in court.”
- Rhode Island: A couple with $400,000 in a bond account became eligible in one month by purchasing “a large single premium immediate annuity.” A single man transferred $100,000 to his son but dodged half of the penalty for transferring assets by using a promissory note to carry out a reverse half-a-loaf strategy.
- Virginia: A man bought a $900,000 annuity in his wife’s name, which paid her $89,000 per month, but “the Virginia Medicaid program could not count this income for purposes of determining the husband’s Medicaid LTC eligibility.”
“Spending down” assets to qualify for Medicaid without expending those funds for LTC or any other health-related expense is far easier and more commonplace than most economists and LTC policy analysts willingly acknowledge.
GOVERNMENT VS. MARKET PRINCIPLES
How Government Impacts Markets in General
This paper first explained how government financing and regulation of LTC, primarily by Medicaid and Medicare, caused the sector’s biggest problems, including institutional bias, inadequate financing, access and quality problems, caregiver shortages, and excessive dependency on unpaid family caregivers. Next the paper described how private sector initiatives mitigated some of the damage done by government, giving examples such as the development of mostly private-pay assisted living, home care, and private insurance. Then it explained how Medicaid dominates LTC, desensitizes the public to this major risk and cost, crowds out potential private financing sources such as insurance or home equity conversion, and so discourages instead of encourages private market solutions that could alleviate LTC’s problems.
What is it about government funding and regulation that causes such problems? Likewise, what is it about private markets that enable them to solve or at least relieve those problems?
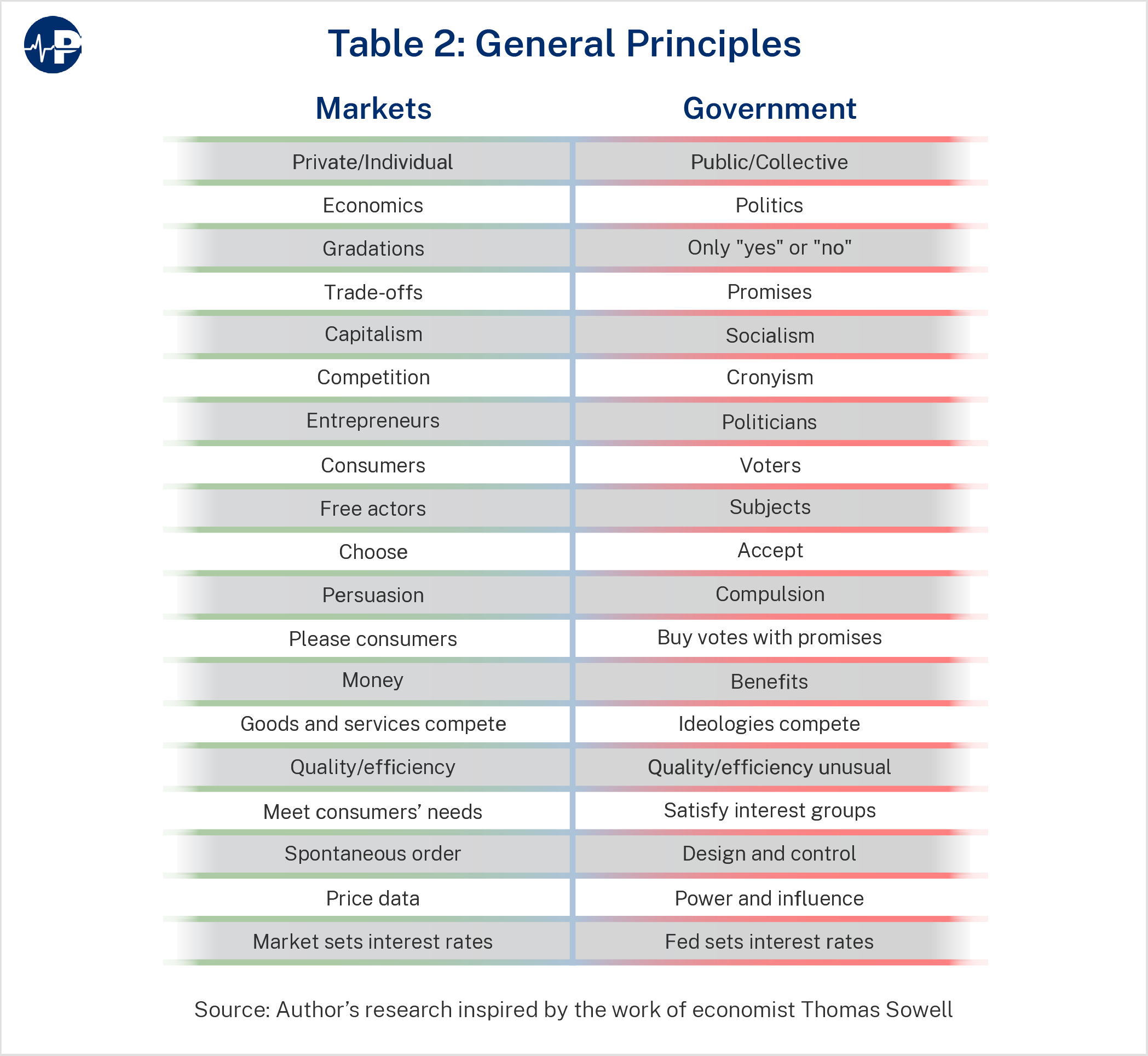
Markets with heavy government involvement, such as the LTC market, operate on different principles than freer markets do. Consider the concepts associated with government compared to parallel notions more commonly related to markets:
- Government evokes politics, politicians, and voters. Markets suggest economics, entrepreneurs, and consumers.
- Government involves interest groups, cronyism, and compulsion. Markets rely on individuals, competition, and persuasion.
- Those who are governed must accept the policies they get from the officials they choose in periodic elections. Market participants continually choose what they want by spending their money in voluntary, mutually beneficial exchanges.
- Governments rely on central planning by powerful elites, often resulting in misallocation of resources, inflation, and shortages of the goods and services people prefer. Markets generate spontaneous order from countless voluntary exchanges, producing price data that tell investors where and how to invest their capital to satisfy people’s needs and wants.
- Government bends toward coercion and socialism. Markets lean toward freedom and capitalism. Their extremes are totalitarianism and anarchy, respectively, so both government and markets must be tempered with good sense, moderation, and, when necessary, litigation.
Furthermore, government and market principles actualize differently. They tend in opposite directions. Government is public, collectivist, and socialistic. Markets are private, individualistic, and capitalistic. Government decisions are made through voting where voters often get only two choices of politicians or ballot measures with no gradations for preference, amount, or quality. In the market, free-acting consumers vote with their cash for (that is, they choose) whatever they want in the quantity and quality they desire. In government, politicians compete by satisfying interest groups with benefits paid for by others, with quality and efficiency notoriously absent. In markets, entrepreneurs compete by creating or identifying and meeting consumers’ needs based on quality and efficiency. In government, the Federal Reserve sets interest rates based on balancing political powers and influence, resulting in asset bubbles, malinvestment, and economic inequality. In markets, millions of transactions among willing buyers and sellers create spontaneous economic order, set interest rates (the price of money) through supply and demand, and generate price data that tell investors and businesses how much of which products and services to produce. Government subjugates; markets liberate.
Is it any wonder, then, that government funding and regulation tend to create economic problems, while markets are inclined to find and implement ways to fix or improve them?
How Economic Principles Express in the LTC Market
Because of the LTC market’s heavy reliance on central planning and government financing, it does not produce the price data investors would need to allocate resources in the most productive and beneficial ways. Medicaid’s dominance of LTC financing compels consumers to adapt to its eligibility and coverage restrictions. It influences providers to supply only such services as Medicaid offers in the quantity and quality it is willing and able to fund. Consequently, U.S. LTC endures access and quality problems; provides too much institutional care and too few HCBS; and suffers caregiver shortages, inadequate public financing, declining private funding, and consumer indifference to planning ahead for future LTC risk and costs. These problems are worse where government prevails in the LTC system and less damaging where markets predominate.
For example, some components of the senior living and LTC markets rely more on public financing and some less. Nursing homes depend most heavily on government financing, especially Medicaid and Medicare. They are the least profitable and the most financially vulnerable sector. Assisted living evolved as a fully private-pay alternative to Medicaid nursing home care, but now one in six assisted living residents receives Medicaid. Specialized memory care in assisted living facilities gets little public funding, but less desirable dementia care in nursing homes receives substantial revenue from Medicare and Medicaid. Home care is heavily financed by government and has more access and quality problems in publicly financed congregate care settings. Independent living is exclusively private pay. By most measures, the more market-based independent and assisted living sectors fare better economically over time than do the more government-dependent nursing home and home health sectors. Profitability—and hence access and quality in the senior housing and care business—is inversely proportional to the level of government funding and regulation.
Conclusion
It behooves analysts and policymakers to consider how public financing created and worsened LTC’s problems before proposing more of the same to fix those problems. The lessons of LTC history are clear: public programs have paid for most expensive LTC since 1965. They diverted the public from responsible LTC planning and left too many people dependent on welfare-financed nursing home care. Easy access to Medicaid LTC financing after expensive care is needed created a moral hazard that discouraged early planning for the risk and cost. The private sector interceded repeatedly with preferred options such as assisted living, private home care, and insurance. But the dominance of Medicaid and Medicare financing for nursing homes prevented alternative modes of LTC service delivery and financing from fully developing based on consumer preferences.
This question remains: Knowing what we know now about the damage government financing has wrought, what are the best policy options going forward? That is the question addressed in Part 2, “Long-Term Care: The Solution.”