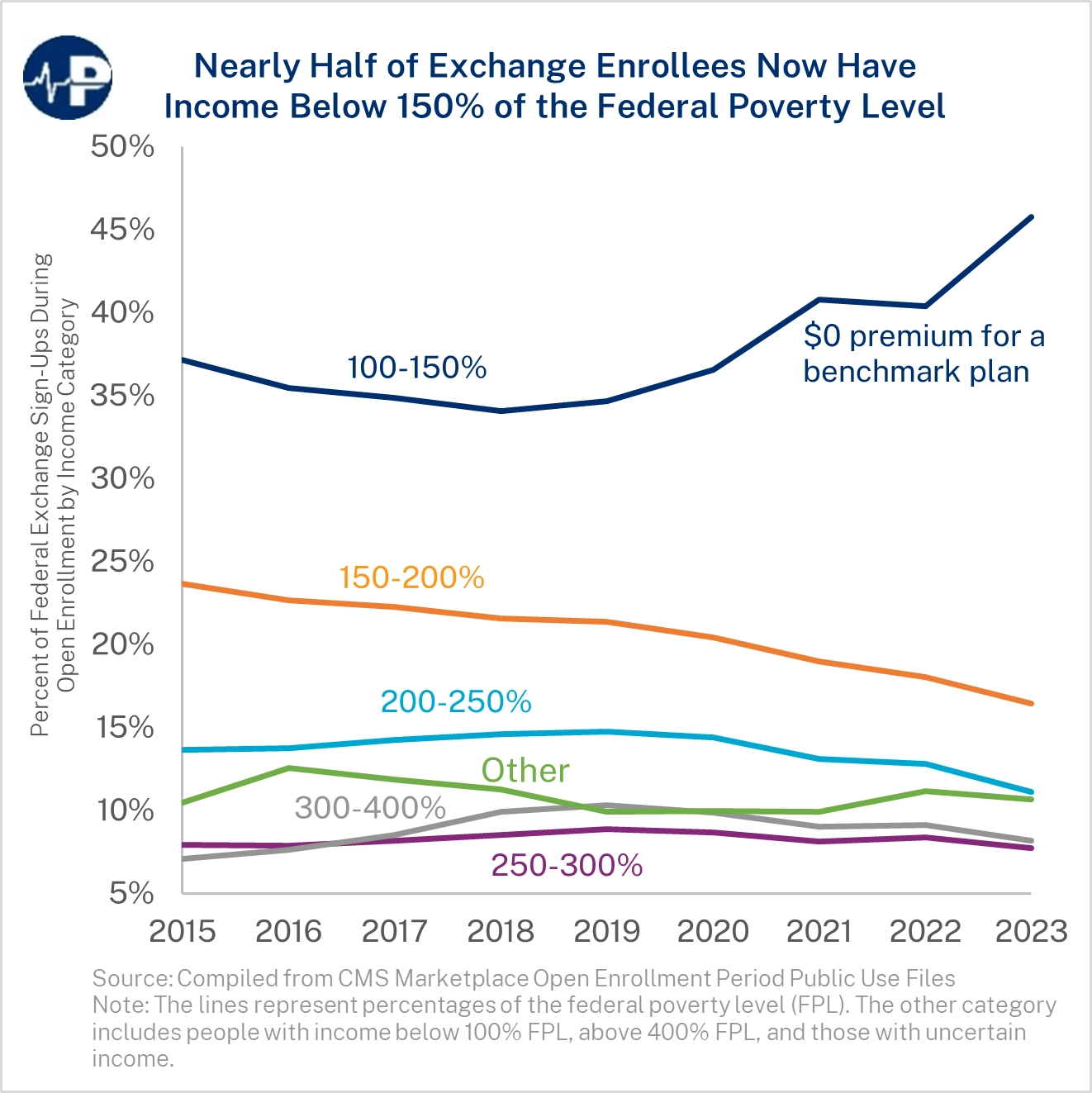
As enrollment data for the 2024 plan year is released, the majority of new enrollment is likely coming from “free” insurance coverage.
The American Rescue Plan Act of 2021 (ARPA) significantly increased subsidies for Affordable Care Act (ACA) exchange plans. The subsidy amount limits the premium people must pay for a benchmark plan (the second lowest-cost silver plan), although the subsidy can be applied to any plan. The subsidies are larger for lower-income people. People below 150 percent of the federal poverty level (FPL) also pay virtually no cost-sharing, including a de minimis deductible, if they select a silver plan.
As a result of ARPA, individuals making under 150 percent of the FPL now pay no premium for a benchmark plan, whereas previously, they had to contribute 2 to 4 percent of their income. These increased subsidies substantially increased exchange enrollment, and it is clear that new enrollment is coming from people who now pay nothing for coverage.
In 2019, roughly 35 percent of people who selected a plan during open enrollment in a state using HealthCare.gov had income between 100-150 percent of the FPL. In 2023, this population accounted for 46 percent of enrollment. The enrollment data by income for the 2024 plan year has yet to be released.
Prior to ARPA, many people below 150 percent of FPL were unwilling to pay the $25 or less per month required to enroll in an ACA plan—a strong sign that they don’t place much value on the coverage.
The main takeaway from ARPA: if people don’t have to pay anything for an ACA plan, they will finally enroll. This seems more an indictment of the ACA than a victory.